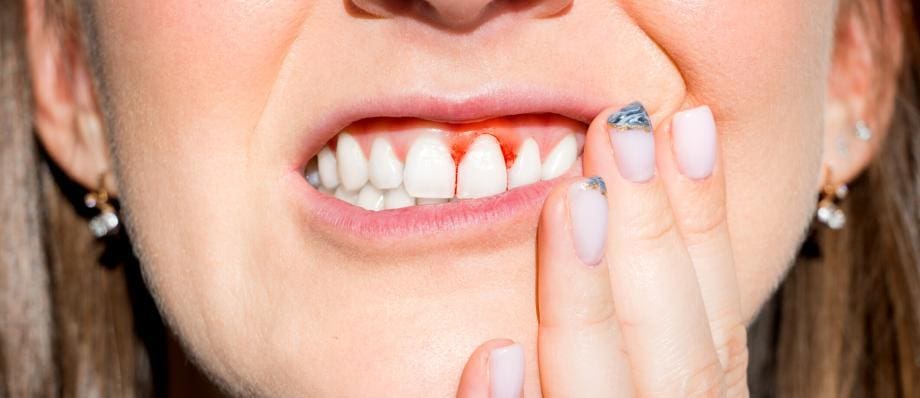
Gingivitis is a common oral health condition characterized by inflammation of the gums. It is the earliest stage of gum disease and, if left untreated, can progress to a more severe condition known as periodontitis. While gingivitis is prevalent, it is also highly preventable and reversible with proper oral hygiene and regular dental care. In this article, we will explore the causes, symptoms, and available treatment options for gingivitis.
Table of Contents
ToggleCauses of Gingivitis
Gingivitis is primarily caused by plaque buildup on the teeth and along the gumline. Plaque is a sticky film composed of bacteria, food particles, and saliva. When plaque is not adequately removed through brushing and flossing, it can harden into tartar (calculus), leading to gum inflammation. Several factors contribute to the development of gingivitis, including:
- Poor oral hygiene
- Hormonal changes
- Medications
- Smoking and tobacco use
- Systemic diseases
- Genetic factors
Poor oral hygiene
Inadequate brushing and flossing allow plaque to accumulate, leading to gum irritation.
Hormonal changes
Hormonal fluctuations during pregnancy, puberty, and menopause can increase the risk of gingivitis.
Medications
Certain medications, such as anticonvulsants and oral contraceptives, can cause gingival overgrowth, making it harder to keep the gums clean.
Smoking and tobacco use
Smoking tobacco products impair blood flow to the gums, making them more susceptible to infection.
Systemic diseases
Conditions like diabetes, HIV/AIDS, and leukemia compromise the immune system, increasing the risk of gum disease.
Genetic factors
Some individuals may have a genetic predisposition to developing gum disease.
Symptoms of Gingivitis
Identifying the symptoms of gingivitis is crucial for early detection and intervention. While gingivitis may be present without causing discomfort, some common signs to watch for include:
- Red and swollen gums
- Bad breath (halitosis)
- Receding gums
- Gum sensitivity
- Changes in gum appearance
Red and swollen gums
Healthy gums are pale pink and firm, but in gingivitis, they appear inflamed, tender, and may bleed easily during brushing or flossing.
Bad breath (halitosis)
The buildup of bacteria and toxins in the mouth can cause persistent bad breath.
Receding gums
Gingivitis can cause the gums to recede or pull away from the teeth, creating gaps or pockets.
Gum sensitivity
The gums may become more sensitive to hot, cold, sweet, or acidic foods and drinks.
Changes in gum appearance
Gingivitis can result in a shiny appearance of the gums due to swelling.
Diagnosis of Gingivitis
Diagnosing gingivitis is typically done through a comprehensive dental examination. Dentists or dental hygienists will assess the gums for signs of inflammation, bleeding, and plaque buildup. They may use instruments to measure pocket depths, indicating the severity of gum disease. Additionally, X-rays may be taken to determine if there is any underlying bone loss.
Prevention of Gingivitis
Preventing gingivitis is crucial to maintaining optimal oral health. The following preventive measures can help reduce the risk of developing this condition:
- Brushing and flossing
- Using an antibacterial mouthwash
- Regular dental check-ups
- Healthy lifestyle choices
Brushing and flossing
Regularly brushing your teeth at least twice a day and flossing once a day helps remove plaque and prevent its buildup.
Using an antibacterial mouthwash
Mouth rinses containing antimicrobial agents can help reduce bacteria and plaque in the mouth.
Regular dental check-ups
Visiting your dentist every six months for professional cleanings and examinations can help identify and treat gingivitis at its earliest stages.
Healthy lifestyle choices
Avoiding tobacco use, maintaining a balanced diet, and managing stress contribute to good oral health.
Treatment Options for Gingivitis
Fortunately, gingivitis is a reversible condition. With appropriate treatment, the gums can return to a healthy state. The treatment options for gingivitis include:
- Professional dental cleaning
- Improved oral hygiene
- Antibacterial mouthwash
- Medications
- Lifestyle modifications
Professional dental cleaning
Scaling and root planing are procedures performed by a dental professional to remove plaque, tartar, and bacteria from above and below the gumline.
Improved oral hygiene
Dentists may provide instructions on proper brushing and flossing techniques and recommend using specialized oral hygiene products.
Antibacterial mouthwash
Mouth rinses containing antimicrobial agents may be prescribed to reduce the bacteria in the mouth and control gingival inflammation.
Medications
In some cases, antibiotics or antimicrobial gels may be prescribed to manage persistent or severe gingivitis.
Lifestyle modifications
Quitting smoking and making healthy lifestyle choices can significantly improve gum health.
Complications of Untreated Gingivitis
If left untreated, gingivitis can progress to a more severe form of gum disease called periodontitis. Periodontitis involves not only inflammation of the gums but also damage to the surrounding tissues and bone that support the teeth. Some potential complications of untreated gingivitis include:
- Periodontal pockets
- Gum recession
- Tooth loss
- Abscess formation
- Systemic health implications
Periodontal pockets
As gingivitis progresses, the gums may pull away from the teeth, forming deep pockets. These pockets provide a space for bacteria to thrive and can lead to further infection and damage.
Gum recession
Advanced gum disease can cause the gums to recede, exposing more of the tooth root. This can lead to tooth sensitivity and an increased risk of tooth decay.
Tooth loss
As periodontitis advances, the supporting tissues and bone can become severely damaged, leading to tooth loss. The weakened foundation can cause teeth to become loose and eventually fall out.
Abscess formation
In some cases, the infection can spread to the deeper tissues, forming a dental abscess. Abscesses are pockets of pus that can cause severe pain and may require immediate dental intervention.
Systemic health implications
Research has found associations between periodontal disease and other health conditions, such as cardiovascular disease, diabetes, respiratory infections, and adverse pregnancy outcomes. While the exact nature of these connections is still being studied, it highlights the importance of maintaining good oral health.
Special Considerations for Treating Gingivitis
Certain groups may require special considerations when it comes to the treatment of gingivitis:
- Pregnancy
- Children and adolescents
- Patients with systemic diseases
Pregnancy
Pregnant women are more prone to gingivitis due to hormonal changes. It is important for expectant mothers to maintain good oral hygiene and visit the dentist regularly for check-ups and cleanings.
Children and adolescents
Proper oral hygiene habits should be instilled early on. Parents should supervise brushing and flossing and ensure regular dental visits for children to prevent and manage gingivitis.
Patients with systemic diseases
Individuals with conditions such as diabetes, HIV/AIDS, or leukemia should work closely with their healthcare providers and dentists to manage their oral health. Controlling these underlying conditions can help reduce the risk and severity of gingivitis.
Promoting Gum Health: Daily Oral Hygiene Practices
In addition to professional dental care, individuals can take proactive measures to promote gum health and prevent gingivitis:
- Brushing technique
- Flossing
- Interdental cleaners
- Mouthwash
- Tongue cleaning
- Balanced diet
Brushing technique
Use a soft-bristle toothbrush and fluoride toothpaste. Brush gently in circular motions, angling the bristles toward the gumline. Be sure to brush all tooth surfaces, including the outer, inner, and chewing surfaces.
Flossing
Flossing helps remove plaque and food particles from between the teeth and along the gumline. Use a gentle sawing motion to guide the floss between teeth, and curve it around each tooth in a C shape to reach beneath the gumline.
Interdental cleaners
If flossing is challenging, interdental cleaners such as interdental brushes or water flossers can be effective alternatives to clean between teeth.
Mouthwash
Incorporate an antimicrobial mouthwash into your oral hygiene routine to reduce plaque and gingival inflammation. Consult with your dentist to determine which mouthwash is best suited for your needs.
Tongue cleaning
Bacteria and viruses can also accumulate on the tongue’s surface, contributing to oral health issues. Gently clean your tongue with a tongue scraper or the back of your toothbrush.
Balanced diet
A nutritious diet rich in vitamins and minerals supports gum health. Limit sugary and acidic foods and beverages, as they can contribute to tooth decay and gum inflammation.
The Role of Dental Professionals
Regular dental visits are crucial for preventing and managing gingivitis. Dental professionals play a vital role in assessing oral health, providing personalized advice, and performing professional cleanings. Here’s what to expect during a dental visit:
- Dental examination
- Professional cleaning
- Oral health education
- Monitoring and follow-up
Dental examination
The dentist or dental hygienist will visually examine your gums, check for signs of inflammation, measure pocket depths, and evaluate overall oral health.
Professional cleaning
Scaling and root planing will be performed to remove plaque, tartar, and bacteria from above and below the gumline. This process helps restore gum health and prevent further damage.
Oral health education
Dental professionals will provide guidance on proper brushing and flossing techniques, recommend suitable oral hygiene products, and answer any questions you may have.
Monitoring and follow-up
For individuals with persistent or severe gingivitis, dental professionals may recommend more frequent visits to monitor progress and adjust treatment as necessary.
Conclusion
Gingivitis is a common and reversible condition that can be effectively managed with proper oral hygiene and regular dental care. By understanding its causes, recognizing the symptoms, and adopting preventive measures, individuals can reduce the risk of developing gingivitis and its complications. Maintaining good gum health is not only essential for oral health but also for overall well-being, as research continues to reveal links between gum disease and systemic health conditions. Remember, your oral health is in your hands, so prioritize consistent oral hygiene practices, schedule regular dental visits, and seek prompt treatment if any signs of gingivitis arise. With a proactive approach, you can preserve healthy gums and maintain a confident smile for years to come.