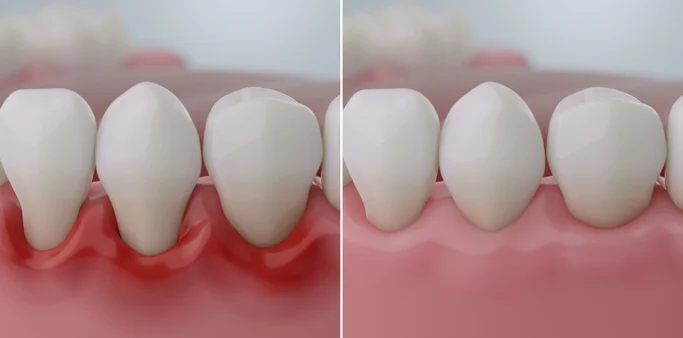
Periodontal diseases are chronic inflammatory conditions affecting the supporting structures of teeth — namely the gingiva, periodontal ligament, cementum, and alveolar bone. When left untreated, these conditions lead to progressive attachment loss, bone resorption, tooth mobility, and eventual tooth loss. The primary goal of periodontal therapy is to eliminate infection, reduce periodontal pockets, and restore a healthy environment conducive to tissue reattachment and regeneration.
While non-surgical periodontal therapy — such as scaling and root planing — forms the foundation of treatment, certain advanced cases necessitate surgical intervention to achieve optimal outcomes. Periodontal surgery provides access for thorough debridement, facilitates the correction of anatomical defects, and enables regeneration of lost structures. Among the various surgical approaches, flap surgeries remain the cornerstone of modern periodontal therapy.
Table of Contents
ToggleThe Modified Widman Flap
Background and Concept
The Modified Widman Flap (MWF) was introduced by Ramfjord and Nissle in 1974 as a refined surgical approach designed to enable open debridement of the root surface with minimal tissue trauma. Unlike older resective techniques that focused on excising pocket walls and reshaping tissues, the MWF emphasizes conservation of soft tissue and gentle management of underlying bone. Its goal is to allow meticulous cleaning of the root surfaces and to promote close adaptation of the gingival flap, thereby reducing the periodontal pocket while preserving esthetics and function.
The hallmark of the modified Widman flap is that it does not attempt to excise the pocket completely, but instead removes a narrow collar of diseased tissue, allowing for healing by long junctional epithelial attachment rather than reattachment of connective tissue fibers.
Surgical Technique
According to the original description by Ramfjord and Nissle (1974), the technique proceeds as follows:
1. Incision Design
- A scalloped internal bevel incision is made parallel to the long axis of the tooth, approximately 1 mm from the gingival margin.
- This first incision removes the pocket epithelium and allows for easier adaptation of the flap upon suturing.
2. Flap Elevation
- The incision is extended interproximally and then extended mesially and distally without vertical relieving incisions.
- The flap is raised as an envelope flap, keeping it conservative and avoiding unnecessary exposure of bone.
3. Secondary Incision (Intercrevicular Incision)
A second incision is made through the bottom of the pocket to detach the collar of granulation tissue and pocket epithelium from the tooth surface.
4. Tertiary Incision (Horizontal Incision)
- A horizontal incision is made at 90° to the tooth, separating the remaining pocket lining.
- The tissue collar is removed using a curette.
5. Debridement
All granulation tissue is removed, and the root surface is meticulously scaled and planed to eliminate bacterial plaque and calculus.
6. Flap Repositioning and Suturing
- The flap is replaced in its original position, closely adapted to the root surface, and sutured without tension.
- Postoperatively, chlorhexidine mouthwash (0.2%) is prescribed twice daily to control plaque.
Healing occurs primarily through the formation of a long junctional epithelial attachment, which seals the pocket and re-establishes a healthy sulcus.
Advantages
- Provides excellent access for root surface debridement.
- Causes minimal trauma to the soft tissues and underlying bone.
- Results in shallow post-operative pocket depth and improved gingival contour.
- Preserves keratinized gingiva, which is important for gingival stability and resistance to mechanical trauma.
- Reduces post-operative discomfort and esthetic complications compared to resective surgeries.
Disadvantages
- Does not aim to remove deep osseous defects; hence, it may not be effective in pockets associated with significant bone loss.
- Some bone exposure may occur, leading to post-operative sensitivity and potential caries risk.
- Healing occurs through long junctional epithelium rather than true new attachment.
- Not ideal for the esthetic zone where gingival recession is a concern.
Clinical Applications
The modified Widman flap is most effective for moderate periodontal pockets (4–6 mm) with limited infrabony defects. It is particularly indicated in cases requiring thorough subgingival debridement but minimal resection of tissue. It remains one of the most commonly taught and performed periodontal flap procedures due to its balance between efficacy and tissue preservation.
The Apically Repositioned Flap
Purpose and Principles
The Apically Repositioned Flap (ARF) is a surgical technique designed to provide greater access to alveolar bone and the root surface while repositioning the gingival margin apically. This results in elimination of the periodontal pocket and lengthening of the clinical crown.
Unlike the MWF, which replaces the flap in its original position, the ARF intentionally repositions the flap apically to expose alveolar bone. This technique is often used when osseous recontouring is required to correct infrabony defects or to perform crown-lengthening procedures for restorative purposes.
Surgical Technique
1. Incision
- A reverse bevel incision is made in the attached gingiva to remove the pocket epithelium and granulation tissue.
- The incision is scalloped to follow the gingival contour, with vertical relieving incisions at either end for better flap mobility.
2. Flap Elevation
- A split-thickness flap is initially raised to preserve the periosteum over the bone.
- The flap is then converted to full thickness as necessary, leaving a collar of tissue around the root surfaces.
3. Debridement and Bone Remodelling
- The granulation tissue and pocket lining are removed with a curette.
- If indicated, osseous recontouring (osteoplasty or ostectomy) is performed to correct irregular bone architecture.
4. Flap Repositioning
The flap is then positioned apically to its original location and sutured in place.
Advantages
- Provides excellent visibility and access for debridement and osseous correction.
- Effective for eliminating deep pockets and establishing a maintainable gingival architecture.
- Useful for crown-lengthening procedures to aid in restorative dentistry.
- Promotes stable gingival margins and reduces the risk of recurrent pocket formation.
Disadvantages
- Post-operative gingival recession may result in root exposure and esthetic concerns.
- Increased risk of root sensitivity and potential for root caries.
- Not suitable for the palatal surfaces, where tissue mobility is limited.
- May compromise the mucogingival junction in cases with thin biotype.
Clinical Applications
The apically repositioned flap is indicated for:
- Shallow to moderate infrabony defects.
- Situations requiring osseous recontouring.
- Crown-lengthening for restorative procedures.
- Pocket elimination in cases of chronic periodontitis.
Osseous Surgery
Definition and Rationale
Osseous surgery refers to surgical reshaping or recontouring of alveolar bone to achieve a physiologic architecture compatible with a healthy periodontium. Although effective, its popularity has declined because bone recontouring inevitably leads to some degree of alveolar resorption and loss of tooth support.
The two primary types of osseous surgery are:
- Osteoplasty – the reshaping of non-supporting bone without removing supporting bone.
- Ostectomy – the removal of supporting bone to eliminate bony defects or irregularities.
Goals of Osseous Surgery
- Eliminate bony ledges, craters, and defects that contribute to pocket formation.
- Establish a smooth, physiologic bone contour that allows for optimal gingival adaptation.
- Facilitate maintenance of the periodontal pocket-free state.
- Improve access for oral hygiene and professional maintenance.
Procedure
Osseous surgery is typically performed in conjunction with flap surgery. After flap reflection and thorough debridement:
- Bone Defect Assessment: The morphology of bone defects is evaluated.
- Resection: Supporting or non-supporting bone is reshaped using hand instruments or rotary burs.
- Smoothing: The bony surface is smoothed to allow the flap to adapt closely to the underlying bone.
- Flap Repositioning: The flap is sutured apically or at the same level depending on the desired gingival margin.
Clinical Considerations
- Osteoplasty should be conservative, maintaining as much supporting bone as possible.
- Ostectomy is indicated when intrabony defects compromise the physiologic bone contour.
- The aim is to restore the correct relationship between bone and tooth, not merely to eliminate pockets.
Limitations
- Inevitably leads to loss of alveolar support.
- May cause post-operative sensitivity, discomfort, and aesthetic compromise.
- Contraindicated in anterior teeth or aesthetic zones due to potential gingival recession.
Other Flap Procedures
The term “other flap procedures” encompasses a range of surgical approaches designed to meet specific clinical goals. These include:
- Simple replaced flaps that provide access for debridement and bone correction without altering the flap position.
- Crown-lengthening procedures, which involve repositioning of the flap apically to increase the clinical crown height for restorative access.
Many clinicians also employ modified flap designs tailored to individual cases, combining principles of MWF and ARF for optimal outcomes. The choice of flap design depends on factors such as pocket depth, bone morphology, gingival thickness, and esthetic demands.
Gingivectomy
Definition and Purpose
Gingivectomy is the surgical excision of diseased gingival tissue to eliminate suprabony periodontal pockets and restore a physiologic gingival contour. Historically, it was one of the earliest periodontal surgical techniques and remains useful in specific cases, particularly where soft-tissue enlargement or fibrous hyperplasia is the primary issue.
Indications
- Persistent supra-alveolar (suprabony) pockets caused by gingival enlargement.
- Gingival hyperplasia due to medications (e.g., phenytoin, cyclosporine, calcium channel blockers).
- Correction of gingival deformities to create a manageable contour.
- Esthetic recontouring in non-bony pocket cases.
It is not suitable for cases involving infrabony pockets because removal of the entire gingival wall would disrupt the biological width and expose the alveolar bone.
Surgical Technique
1. Pocket Marking:
Pockets are delineated using pocket marking forceps such as Crane-Kaplan forceps to identify the pocket base.
2. Incision:
- A beveled incision is made at a 100–110° angle to the long axis of the tooth.
- The incision removes the pocket wall and allows for gingival recontouring.
3. Tissue Removal:
The excised tissue is removed, and the underlying granulation tissue is debrided.
4. Root Surface Preparation:
Root surfaces are planed, and remaining granulation tissue is curetted away.
5. Post-Operative Care:
- A periodontal dressing is applied for approximately one week.
- Chlorhexidine mouthwash (10 mL twice daily) is recommended for plaque control.
Advantages
- Simple and quick technique requiring minimal equipment.
- Provides immediate pocket elimination.
- Useful in cases of drug-induced gingival overgrowth or pseudopockets.
Disadvantages
- Results in loss of attached gingiva, exposing root surfaces and creating sensitivity.
- Healing by secondary intention can cause discomfort and slower recovery.
- Not suitable in esthetic areas due to gingival recession.
- Does not address underlying bone defects or infrabony pockets.
Healing and Post-Operative Considerations
Healing following periodontal surgery depends on the type of procedure performed:
- Modified Widman flap: Healing primarily by long junctional epithelium.
- Apically repositioned flap: Healing involves reattachment of connective tissue fibers and bone remodeling.
- Gingivectomy: Healing by secondary intention with epithelial proliferation from wound margins.
- Osseous surgery: Bone remodeling occurs over several months, with soft tissue adaptation within 4–6 weeks.
Post-operative care includes:
- Use of chlorhexidine mouthwash (0.2%) twice daily.
- Avoidance of mechanical plaque removal near the surgical site for 7–10 days.
- Suture removal typically after 7–10 days.
- Maintenance of good oral hygiene and regular recall visits.
Modern Trends in Periodontal Surgery
In recent years, the focus of periodontal surgery has shifted from resective to regenerative and minimally invasive techniques. Modern approaches aim to preserve tissue and stimulate regeneration rather than simply reduce pocket depth.
Some advancements include:
- Microsurgical flap techniques for better visualization and reduced trauma.
- Guided tissue regeneration (GTR) using barrier membranes to promote new attachment.
- Use of biomaterials such as bone grafts, enamel matrix derivatives, and growth factors to enhance healing.
- Laser-assisted flap surgery, offering precision and improved hemostasis.
These innovations have expanded the scope of periodontal therapy, allowing clinicians to achieve improved functional and esthetic results with fewer complications.
Conclusion
Periodontal flap surgery represents a crucial component of comprehensive periodontal therapy. Each surgical technique — from the conservative Modified Widman Flap to the more extensive Apically Repositioned Flap and Osseous Surgery — has specific indications, advantages, and limitations.
A thorough understanding of tissue biology, flap design, and healing dynamics is essential for achieving optimal outcomes. While traditional procedures remain relevant, the evolution of regenerative and minimally invasive approaches continues to redefine the future of periodontal surgery.
Ultimately, the choice of technique should be guided by the extent of disease, esthetic considerations, and the patient’s overall needs, with the overarching goal of restoring and maintaining a healthy, functional, and aesthetically pleasing periodontium.
References
- Ramfjord, S. P., & Nissle, R. R. (1974). The modified Widman flap. Journal of Periodontology, 45(8), 601–607.
- Lindhe, J., Lang, N. P., & Karring, T. (2015). Clinical Periodontology and Implant Dentistry (6th ed.). Wiley-Blackwell.
- Carranza, F. A., & Newman, M. G. (2019). Carranza’s Clinical Periodontology (13th ed.). Elsevier.
- Cohen, E. S. (2010). Atlas of Cosmetic and Reconstructive Periodontal Surgery (3rd ed.). BC Decker Inc.
- Takei, H. H., Azzi, R. A., & Han, T. J. (2012). Periodontal plastic and esthetic surgery. In Newman, M. G., Takei, H. H., Klokkevold, P. R., & Carranza, F. A. (Eds.), Carranza’s Clinical Periodontology (11th ed., pp. 823–868). Elsevier Saunders.
- Goldman, H. M., & Cohen, D. W. (1958). The infrabony pocket: Classification and treatment. Journal of Periodontology, 29(4), 272–291.
- Waerhaug, J. (1978). Healing of the dento-epithelial junction following subgingival plaque control. Journal of Periodontology, 49(3), 119–134.
- Heitz-Mayfield, L. J. A. (2005). How effective is surgical therapy compared with nonsurgical debridement? Periodontology 2000, 37(1), 72–87.
- Cortellini, P., & Tonetti, M. S. (2015). Clinical concepts for regenerative therapy in intrabony defects. Periodontology 2000, 68(1), 282–307.
- Greenwell, H., Fiorellini, J. P., Giannobile, W. V., Offenbacher, S., Salkin, L., Townsend, C., … & Committee on Research, Science and Therapy, American Academy of Periodontology. (2005). Oral reconstructive and corrective considerations in periodontal therapy. Journal of Periodontology, 76(9), 1588–1600.
- Kornman, K. S., & Robertson, P. B. (2000). Clinical and microbiological evaluation of periodontal therapy. Periodontology 2000, 22(1), 41–58.
- Bouchard, P., Malet, J., & Borghetti, A. (2001). Decision-making in aesthetics: Root coverage revisited. Periodontology 2000, 27(1), 97–120.
- Trombelli, L., Farina, R., Silva, C. O., & Tatakis, D. N. (2018). Plaque-induced gingivitis: Case definition and diagnostic considerations. Journal of Clinical Periodontology, 45(S20), S44–S67.
- Sculean, A., Chapple, I. L. C., Giannobile, W. V., & Tonetti, M. S. (2019). Periodontology 2000: Evidence-based advances in periodontology and implant dentistry. Wiley-Blackwell.