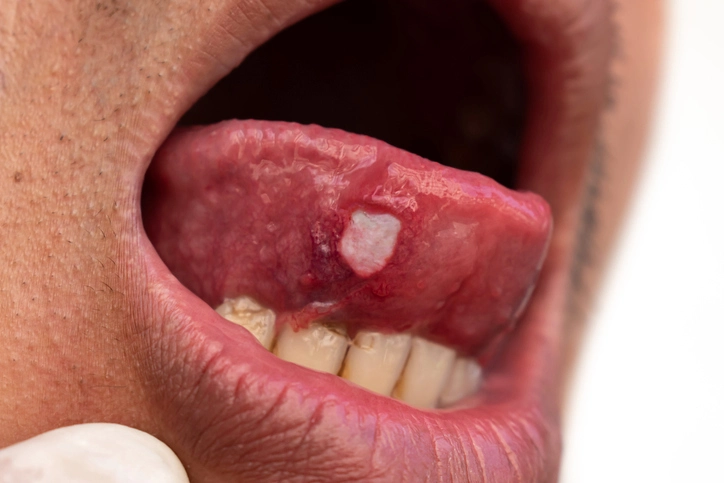
The oral cavity is uniquely vulnerable to adverse drug reactions because it is continuously exposed to medications both systemically and locally. Drugs may reach the oral tissues directly through topical application, accidental contact, or ingestion, and indirectly via systemic circulation. As a result, the mouth often serves as an early indicator of drug toxicity, hypersensitivity, or systemic adverse effects.
Drug-induced lesions of the mouth encompass a wide spectrum of clinical presentations ranging from mild discomfort and reversible mucosal changes to severe ulceration, infections, and life-threatening mucocutaneous syndromes. Recognition of these lesions is essential for dentists, physicians, and other healthcare professionals, as early diagnosis can prevent unnecessary morbidity and guide appropriate modification of therapy.
For educational clarity, drug-induced oral lesions are commonly divided into local reactions and systemic effects.
Table of Contents
ToggleClassification of Drug-Induced Oral Lesions
Drug-induced oral lesions can broadly be categorized as:
- Local reactions – resulting from direct contact of a drug with the oral tissues
- Systemic effects – resulting from systemic drug action affecting oral structures
This distinction aids in diagnosis and helps guide management strategies.
Local Reactions
1. Chemical Burns of the Oral Mucosa
Pathogenesis
Chemical burns of the oral mucosa occur due to direct contact between a corrosive or irritant substance and the oral tissues. One classic example is the placement of an aspirin tablet against the gingiva or buccal mucosa adjacent to a painful tooth. Although this practice is discouraged, it continues to be encountered in clinical practice.
Aspirin (acetylsalicylic acid) causes localized tissue necrosis due to its acidic nature. The damage is usually superficial, affecting the epithelial layer, but may extend deeper with prolonged exposure.
Iatrogenic chemical burns may occur during dental procedures, particularly from:
- Trichloroacetic acid
- Sodium hypochlorite
- Phenol
Accidental ingestion of corrosive substances such as paraquat can also produce severe oral and systemic injury.
Clinical Features
- White, sloughing patches on the mucosa
- Pain or burning sensation
- Erythema surrounding the lesion
- In severe cases, ulceration
The lesion may initially appear alarming but is typically transient if the irritant is removed promptly.
Management
- Immediate removal of the offending agent
- Patient education to prevent recurrence
- Symptomatic treatment (e.g., topical anesthetics)
- Reassurance, as spontaneous healing usually occurs
2. Interference with Commensal Oral Flora
Pathogenesis
The oral cavity hosts a complex ecosystem of microorganisms that maintain mucosal health. Prolonged or repeated use of antibiotics—particularly topical antibiotics—can disrupt this balance by suppressing normal bacterial flora. This creates an environment favorable for opportunistic organisms, especially Candida species.
Corticosteroids, whether inhaled or systemic, further exacerbate this risk by causing immunosuppression.
Clinical Features
- Oral candidiasis (thrush)
- White, creamy plaques that can be wiped off
- Erythematous or atrophic mucosa
- Burning sensation or altered taste
Management
- Identification and modification of the causative drug, if possible
- Antifungal therapy (topical or systemic)
- Reinforcement of oral hygiene measures
- Rinsing mouth after inhaled steroid use
3. Oral Dysaesthesia
Pathogenesis
Oral dysaesthesia refers to abnormal oral sensations without obvious clinical pathology. Certain drugs may affect neural transmission or local blood flow, resulting in sensory disturbances.
Captopril, an angiotensin-converting enzyme (ACE) inhibitor, is a recognized cause.
Clinical Features
- Burning or sore tongue
- Normal clinical appearance
- Symptoms may be persistent or intermittent
Management
- Exclusion of other causes (e.g., nutritional deficiencies, infections)
- Review of medication history
- Drug substitution where feasible
Systemic Effects
1. Depressed Bone Marrow Function
Pathogenesis
Many drugs affect hematopoiesis, leading to reduced production of red cells, white cells, or platelets. These changes can have significant oral manifestations due to impaired immunity, oxygen delivery, and clotting mechanisms.
Drugs commonly implicated include:
- Phenytoin
- Chloramphenicol
- Certain analgesics
Long-term use of some medications can result in folate deficiency and macrocytic anemia, further compromising mucosal integrity.
Clinical Features
- Severe aphthous-like ulceration
- Persistent oral ulcers
- Increased susceptibility to infection
- Petechiae, purpura, or bleeding (rare)
Agranulocytosis may present with rapidly progressing, painful ulcers due to lack of neutrophil-mediated defense.
Management
- Urgent medical evaluation
- Blood investigations
- Discontinuation of the offending drug where possible
- Supportive oral care to prevent secondary infection
2. Immunosuppression-Related Oral Disease
Pathogenesis
Immunosuppressive drugs such as corticosteroids and azathioprine reduce immune surveillance and resistance to infection. This predisposes patients to opportunistic viral and fungal infections.
Clinical Features
- Recurrent oral candidiasis
- Herpetic infections
- Poor wound healing
- Chronic mucosal inflammation
Management
- Vigilant monitoring of oral health
- Early treatment of infections
- Patient education regarding oral hygiene
3. Lichenoid Drug Reactions
Pathogenesis
Drug-induced lichenoid reactions resemble oral lichen planus both clinically and histologically. The reaction is believed to be immune-mediated.
Gold therapy for rheumatoid arthritis is classically associated, but many commonly prescribed drugs may also trigger these lesions, including:
- NSAIDs
- Oral hypoglycaemic agents
- Beta-blockers
Clinical Features
- White striations (Wickham-like lines)
- Erythematous or ulcerated areas
- Bilateral or unilateral presentation
- Burning or discomfort
Management
- Differentiation from idiopathic lichen planus
- Withdrawal or substitution of the offending drug when feasible
- Topical corticosteroids for symptom relief
4. Erythema Multiforme and Stevens–Johnson Syndrome
Pathogenesis
Erythema multiforme is a hypersensitivity reaction that may progress to Stevens–Johnson syndrome, a severe and potentially life-threatening condition. Drugs are a major trigger.
Clinical Features
- Widespread oral ulceration
- Hemorrhagic crusting of lips
- Skin target lesions
- Systemic symptoms such as fever
Management
- Immediate medical referral
- Discontinuation of causative drug
- Supportive care in a hospital setting
5. Exfoliative Stomatitis
Pathogenesis
Exfoliative stomatitis represents the oral manifestation of exfoliative dermatitis, a severe adverse drug reaction characterized by widespread epithelial shedding.
Gold therapy has again been implicated.
Clinical Features
- Sloughing of oral mucosa
- Painful erosions
- Difficulty eating and speaking
Management
- Medical emergency
- Withdrawal of offending agent
- Supportive multidisciplinary care
6. Gingival Hyperplasia
Pathogenesis
Drug-induced gingival enlargement is caused by increased fibroblast activity and collagen production. It is most commonly associated with:
- Phenytoin
- Ciclosporin
- Nifedipine and other calcium channel blockers
- Occasionally oral contraceptive pills
Poor oral hygiene exacerbates the condition, although gingival enlargement may occur even with meticulous plaque control.
Clinical Features
- Firm, fibrous gingival overgrowth
- Difficulty maintaining oral hygiene
- Aesthetic concerns
- Increased risk of periodontal disease
Management
- Meticulous oral hygiene instruction
- Review of drug therapy
- Surgical gingivectomy in severe cases
Other Drug-Induced Oral Manifestations
Oral Pigmentation
- Heavy metal poisoning causes black lines in the gingival sulcus
- Chlorhexidine causes brown or black discoloration of the tongue
- Tetracycline causes intrinsic tooth discoloration
Xerostomia
Many drugs reduce salivary flow, leading to dry mouth, increased caries risk, and mucosal discomfort.
Allergic Reactions
Penicillin is a common cause of oral allergic reactions, which may include swelling, erythema, or ulceration.
Clinical Approach and Conclusion
Drug-induced oral lesions require a careful and systematic approach:
- Detailed medical and drug history
- Recognition of characteristic patterns
- Collaboration with prescribing physicians
- Balancing oral health with systemic therapeutic needs
In some cases, withdrawal of the offending drug is possible. In others, minor oral symptoms may need to be tolerated when the medication is essential for the patient’s overall well-being.
In conclusion, awareness of drug-induced oral lesions is vital for early diagnosis, prevention of complications, and optimal patient care. The oral cavity remains a valuable window into systemic drug reactions, reinforcing the importance of interdisciplinary collaboration in healthcare.