Teeth grinding, medically known as bruxism, is a prevalent condition characterized by the involuntary clenching and grinding of teeth. This behavior can occur during wakefulness or sleep, leading to various dental and muscular complications. Traditional treatments have ranged from dental appliances to behavioral therapies. However, recent advancements have introduced botulinum toxin (commonly known as Botox) as a potential therapeutic option. This article delves into the application of botox in treating bruxism, exploring its mechanisms, efficacy, benefits, and considerations.
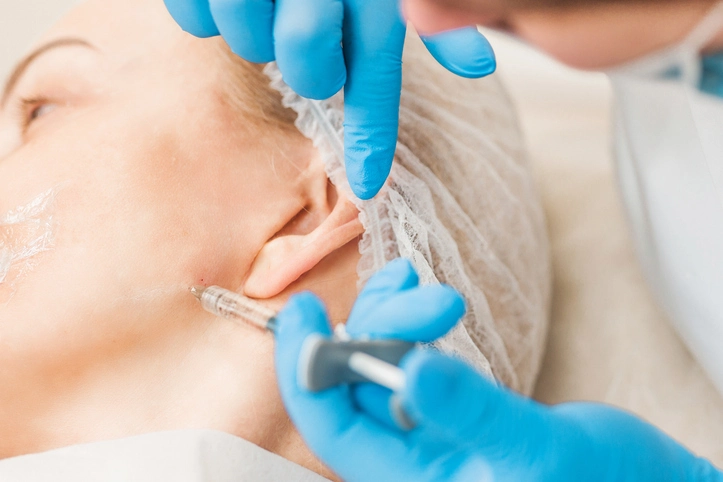
Table of Contents
ToggleUnderstanding Bruxism
Bruxism is a condition characterized by the repetitive and involuntary grinding, gnashing, or clenching of teeth. It can occur either during wakefulness or sleep and may go unnoticed for a long time until noticeable symptoms or complications emerge. Bruxism is increasingly recognized as a multifactorial disorder with both physical and psychological components, affecting both children and adults across all age groups.
Types of Bruxism
Bruxism is commonly categorized into two main types based on when it occurs:
- Awake Bruxism (Diurnal Bruxism)
- Sleep Bruxism (Nocturnal Bruxism)
Awake Bruxism (Diurnal Bruxism)
Typically occurs during the day, especially during periods of concentration, stress, anxiety, or frustration. It usually involves conscious or semi-conscious jaw clenching without tooth grinding. Often associated with poor posture, occupational stress, or habitual behaviors like chewing on pens or nails.
Sleep Bruxism (Nocturnal Bruxism)
Occurs during sleep and is considered a sleep-related movement disorder. It may be rhythmic (phasic) or sustained (tonic) in nature, and individuals are usually unaware they are grinding their teeth unless informed by a partner or noted by a dentist.
Sleep bruxism is more likely to be associated with arousals from sleep, and it may co-exist with other sleep disorders like sleep apnea.
Causes and Contributing Factors
While the exact cause of bruxism is not fully understood, it is widely believed to result from a combination of physical, psychological, and genetic factors.
1. Psychological Factors
- Stress and Anxiety: One of the most significant contributors to both awake and sleep bruxism.
- Emotional Stress: High emotional reactivity, irritability, and suppressed anger have been associated with bruxism.
- Mental Health Disorders: Depression, general anxiety disorder, and obsessive-compulsive tendencies can elevate risk.
2. Sleep-Related Issues
- Obstructive Sleep Apnea (OSA): A common co-existing condition in individuals with sleep bruxism.
- Arousals During Sleep: Increased micro-arousals can stimulate masticatory muscle activity.
- Insomnia and Sleep Disruption: Individuals with fragmented or poor-quality sleep are at higher risk.
3. Dental and Jaw-Related Factors
- Malocclusion: Misalignment of the teeth or jaw may play a role, although its significance is debated.
- Tooth Anatomy and Bite Force: Certain jaw shapes and bite forces may predispose people to bruxism.
4. Medications and Substances
- Antidepressants: Especially SSRIs (e.g., fluoxetine, sertraline) have been associated with an increased risk of bruxism.
- Stimulants: Caffeine, nicotine, and illicit drugs like cocaine and MDMA (ecstasy) can exacerbate bruxism.
- Alcohol Consumption: May increase muscle activity during sleep and worsen bruxism.
5. Genetic Predisposition
Bruxism tends to run in families, suggesting a hereditary component. First-degree relatives of bruxers are more likely to exhibit the behavior themselves.
Traditional Treatment Approaches
Before botulinum toxin (Botox) emerged as a clinical treatment for bruxism, a variety of traditional methods were used — and still are — to manage the condition. These conventional therapies aim to reduce the physical damage caused by grinding and clenching, alleviate associated symptoms such as pain or headaches, and in some cases, address underlying causes like stress or malocclusion.
While some of these treatments provide temporary or partial relief, others can be effective for long-term management when tailored to the patient’s needs. Let’s take a closer look at the primary traditional treatment strategies:
- Occlusal Splints and Night Guards
- Behavioral and Stress Management Techniques
- Pharmacological Interventions
- Dental Corrections and Orthodontics
- Physical Therapy and Massage
- Lifestyle and Habit Modification
Occlusal Splints and Night Guards
One of the most widely used interventions for bruxism, occlusal splints (commonly known as night guards or bite guards) are custom-fitted dental appliances made from soft or hard acrylic material. They are worn over the teeth, usually during sleep, to prevent direct tooth-on-tooth contact and protect against wear and fractures.
Types:
- Soft Night Guards: Flexible and usually prescribed for mild bruxism.
- Hard Night Guards: More durable and designed for severe grinders or clenchers.
- Dual Laminate Guards: Combine a soft inner layer with a hard exterior for comfort and protection.
Pros:
- Protects teeth from damage.
- Non-invasive and relatively affordable.
- Easily customized for individual needs.
Cons:
- Does not stop the grinding behavior itself.
- May need frequent adjustments or replacements.
- Can be uncomfortable for some, leading to poor compliance.
Behavioral and Stress Management Techniques
Since psychological stress and anxiety are common triggers for bruxism, particularly awake bruxism, behavioral strategies can play a key role in management. These interventions focus on reducing stress, increasing awareness of jaw clenching habits, and modifying behavior.
Examples:
- Cognitive Behavioral Therapy (CBT): Helps identify and change thought patterns and behaviors associated with stress and bruxism.
- Biofeedback: Uses electronic monitoring to help patients become aware of jaw muscle activity and learn to control it consciously.
- Relaxation Techniques: Includes meditation, breathing exercises, progressive muscle relaxation, and yoga to manage stress.
Pros:
- Addresses the root psychological causes of bruxism.
- Can reduce frequency and intensity of clenching or grinding.
- Non-invasive and free of side effects.
Cons:
- Results may take time and require consistent practice.
- May not be effective as a standalone treatment in severe cases.
- Availability of trained practitioners can be limited.
Pharmacological Interventions
In certain cases, medications may be used to manage bruxism, especially when it’s linked to other medical or psychological conditions. These are generally considered secondary options due to side effects and limited long-term effectiveness.
Common Medications:
- Muscle Relaxants: Prescribed short-term to reduce muscle activity and relieve pain.
- Benzodiazepines (e.g., clonazepam): Sometimes used for short-term sleep bruxism, especially when associated with insomnia or anxiety.
- Antidepressants or Anti-anxiety Medications: May be prescribed if bruxism is tied to depression or generalized anxiety disorder.
- Botulinum Toxin (Botox): Though newer, some may consider this an advanced pharmacological approach (discussed in the main article body).
Pros:
- Can offer temporary symptom relief.
- Helpful in managing comorbid conditions (e.g., anxiety, depression, insomnia).
Cons:
- Risk of dependency (especially with benzodiazepines).
- Side effects can outweigh benefits for some.
- Does not directly address the mechanical effects on the teeth and jaw.
Dental Corrections and Orthodontics
In cases where bruxism is believed to be aggravated by malocclusion (improper alignment of teeth), dental interventions may be recommended. These can range from minor adjustments to full orthodontic treatment.
Examples:
- Selective Occlusal Adjustment: Minor reshaping of enamel to improve bite alignment.
- Orthodontic Treatment: Braces or aligners to correct jaw or bite positioning.
- Dental Restorations: Crowns or overlays used to restore damaged teeth and reestablish functional occlusion.
Pros:
- May reduce mechanical triggers of bruxism.
- Improves long-term oral health and functionality.
- Can restore damaged dentition.
Cons:
- Invasive and may be expensive.
- Evidence linking occlusal correction to long-term bruxism improvement is mixed.
- May not help if bruxism is primarily stress-related or neurologically based.
Physical Therapy and Massage
Physical therapy approaches, particularly for chronic or painful bruxism, involve exercises and manual therapies to alleviate muscle tension, improve range of motion, and reduce TMJ (temporomandibular joint) discomfort.
Examples:
- Myofascial Release and Massage Therapy: Targeting the masseter, temporalis, and other jaw muscles to relieve tension.
- Jaw Exercises: Designed to strengthen and relax the jaw and surrounding muscles.
- Heat and Cold Therapy: To reduce inflammation and muscle soreness.
Pros:
- Non-invasive, drug-free approach.
- Can be used in combination with other therapies.
- Especially beneficial for patients with TMD symptoms.
Cons:
- Requires multiple sessions over time.
- Relief may be temporary without addressing underlying causes.
- Effectiveness can vary depending on practitioner expertise.
Lifestyle and Habit Modification
Simple changes in daily behavior and routines can significantly impact the severity of bruxism. Patients are often advised to avoid habits that put strain on the jaw and to adopt practices that promote jaw relaxation.
Recommendations Include:
- Avoid chewing gum or non-food items (pens, fingernails).
- Practice maintaining proper jaw posture (lips closed, teeth apart).
- Use warm compresses on the jaw before bed.
- Reduce consumption of caffeine and alcohol, especially in the evening.
- Get adequate, quality sleep.
Pros:
- Cost-effective and accessible.
- Encourages patient responsibility and awareness.
- Can significantly reduce awake bruxism symptoms.
Cons:
- Requires motivation and consistency.
- Less effective for severe or sleep-related bruxism on its own.
Botulinum Toxin: An Overview
Botulinum toxin — most commonly recognized under the brand name Botox — is a powerful neurotoxic protein produced by the bacterium Clostridium botulinum. While it is infamous for causing botulism, a rare and potentially fatal illness, in controlled clinical settings, it has become a valuable and versatile tool in both cosmetic and therapeutic medicine.
What makes botulinum toxin unique is its ability to block nerve signals to muscles, leading to temporary muscle relaxation or paralysis. This action has been harnessed to treat a wide variety of conditions, ranging from facial wrinkles to chronic migraines, muscle spasticity, excessive sweating, and, increasingly, bruxism.
History and Development of Botulinum Toxin in Medicine
Botulinum toxin has a fascinating trajectory — from feared toxin to medical marvel.
- Early Discovery: In the early 19th century, botulism was first described as a foodborne illness related to improperly stored meats. The toxin responsible was isolated in the late 19th century by Emile van Ermengem.
- First Therapeutic Use: The medical potential of the toxin was realized in the 1970s. Dr. Alan Scott, an ophthalmologist, began using it to treat strabismus (crossed eyes) by injecting small, diluted amounts into eye muscles. This led to the first FDA-approved medical use of botulinum toxin in the 1980s.
- Cosmetic Breakthrough: In 2002, the FDA approved Botox Cosmetic for the temporary reduction of glabellar lines (frown lines between the eyebrows), sparking global interest in its aesthetic uses.
- Expansion into Neurology, Pain, and Muscular Disorders: Since then, botulinum toxin has been approved for a growing list of indications — including cervical dystonia, spasticity, hyperhidrosis, chronic migraines, overactive bladder, and bruxism.
Today, botulinum toxin comes in several formulations, including:
- Botox (onabotulinumtoxinA)
- Dysport (abobotulinumtoxinA)
- Xeomin (incobotulinumtoxinA)
- Jeuveau, Myobloc, and others
Each formulation has slightly different molecular weights, diffusion properties, and storage requirements, but all work on the same fundamental principle.
How Botulinum Toxin Works
The primary mechanism of botulinum toxin is neuromuscular blockade. Here’s how it works at the molecular level:
- Binding: The toxin binds to presynaptic cholinergic nerve terminals at the neuromuscular junction — the point where motor neurons communicate with muscle fibers.
- Internalization: Once bound, the toxin is internalized into the nerve cell via endocytosis.
- Cleavage of SNARE Proteins: The active component of the toxin cleaves specific proteins (such as SNAP-25, synaptobrevin, or syntaxin) that are essential for the release of acetylcholine — the neurotransmitter responsible for muscle contraction.
- Inhibition of Acetylcholine Release: By preventing acetylcholine from being released into the synaptic cleft, the toxin effectively “shuts down” muscle activation at that site.
- Temporary Paralysis: The muscle becomes weak or paralyzed for a period ranging from 3 to 6 months, depending on the dose and individual response.
Why Botulinum Toxin for Bruxism?
Bruxism is characterized by overactivity of the masticatory muscles, especially the masseter, temporalis, and sometimes the medial pterygoid. Unlike treatments that merely protect the teeth (e.g., night guards) or target behavioral triggers, botulinum toxin directly addresses the muscle hyperactivity itself.
By selectively weakening these overactive muscles:
- The intensity and frequency of grinding/clenching is reduced.
- Pain from muscle fatigue or temporomandibular joint strain is alleviated.
- In chronic cases, the hypertrophied masseter muscle can visibly reduce in size, improving facial contour.
Importantly, botulinum toxin does not paralyze the muscles completely when administered in appropriate therapeutic doses — rather, it reduces excessive contraction, allowing normal function (e.g., chewing, speaking) to continue with fewer symptoms.
Mechanism of Action in Bruxism Treatment
In bruxism management, botulinum toxin is injected into the masticatory muscles, primarily the masseter and temporalis muscles. By partially paralyzing these muscles, the toxin reduces their strength and activity, thereby diminishing the intensity of teeth grinding and clenching. This reduction alleviates muscle hypertrophy, decreases pain, and minimizes dental damage associated with bruxism.
How Botox Works in the Context of Bruxism
Here’s a step-by-step breakdown of how botulinum toxin alters muscle activity in the context of bruxism:
Step 1: Neuromuscular Blockade
Once injected into the muscle, botulinum toxin binds to cholinergic nerve terminals — the nerve endings that communicate with muscle fibers.
Step 2: Acetylcholine Inhibition
The toxin cleaves SNARE proteins (specifically SNAP-25, a key molecule in neurotransmitter release), preventing the release of acetylcholine, the chemical messenger that stimulates muscle contraction.
Step 3: Reduced Muscle Contraction
Without acetylcholine, the affected muscle cannot receive the “contract” signal from the brain. The result is a temporary weakening of the muscle — it can still function, but with reduced strength and frequency of contraction.
Step 4: Reduced Grinding and Clenching
As the masseter and other jaw muscles become less powerful, the patient grinds and clenches less intensely — or may stop altogether during sleep or moments of stress.
Step 5: Symptom Relief
This leads to a cascade of benefits:
- Decreased tooth wear and enamel damage
- Reduced jaw pain and facial tension
- Improvement in temporomandibular joint (TMJ) dysfunction
- Fewer headaches and morning jaw stiffness
- Aesthetic softening of an overly prominent jawline in cases of masseter hypertrophy
Onset and Duration of Action
- Onset: Patients typically begin to notice effects within 3 to 7 days of injection.
- Peak Effect: Around 2 to 4 weeks post-injection.
- Duration: Relief lasts approximately 3 to 6 months, depending on dosage, individual metabolism, and severity of bruxism. Repeat treatments are often necessary to maintain results.
Efficacy of Botulinum Toxin in Bruxism
Several studies have investigated the effectiveness of botulinum toxin in treating bruxism:
- Pain Reduction: Research indicates that botulinum toxin injections can significantly reduce pain levels associated with bruxism. A study published in the Journal of Pain Research found that botulinum toxin type A (BTX-A) led to a notable decrease in bruxism-induced pain compared to placebo or conventional treatments.
- Decrease in Bruxism Episodes: Clinical trials have demonstrated that BTX-A injections can reduce the frequency of bruxism episodes. For instance, a systematic review highlighted that patients receiving botulinum toxin experienced fewer grinding events during sleep.
- Muscle Activity Reduction: Electromyographic assessments have shown decreased muscle activity in the masseter and temporalis muscles following botulinum toxin treatment, indicating effective muscle relaxation.
While these findings are promising, it’s essential to note that responses can vary among individuals, and further large-scale studies are needed to establish standardized protocols.
Procedure and Dosage
The use of botulinum toxin (commonly referred to as Botox) for bruxism requires precise technique, a strong understanding of facial anatomy, and individualized treatment planning. Since the therapy involves the temporary weakening of overactive jaw muscles, it’s essential to ensure both effectiveness and safety by administering the right dosage at the correct anatomical locations.
Let’s explore how the procedure is performed, from consultation to post-treatment care.
1. Pre-Treatment Evaluation
Before administering botulinum toxin for bruxism, a comprehensive clinical assessment is crucial.
Key steps include:
Medical History Review
The clinician checks for any contraindications, such as neuromuscular disorders (e.g., myasthenia gravis), allergies to botulinum toxin components, pregnancy, or use of aminoglycoside antibiotics, which may enhance toxin effects.Bruxism Assessment
This includes a detailed history of the patient’s bruxism pattern (sleep vs. awake bruxism), symptom severity, triggers (e.g., stress, medications), and previous treatments.Muscle Examination
Palpation of the masseter, temporalis, and possibly medial pterygoid muscles to assess:Muscle tone and tenderness
Degree of hypertrophy (overdevelopment)
Asymmetry in jawline or bite
Pain during movement or clenching
Dental Evaluation
Identification of tooth wear, enamel fractures, TMJ dysfunction, and bite misalignment helps guide the decision to combine Botox with other dental treatments (like night guards or occlusal correction).
2. Injection Sites and Technique
The injection technique is tailored based on the patient’s anatomy and severity of bruxism. The most common muscles treated are:
Masseter Muscle
- Location: At the angle of the jaw, palpable when the patient clenches their teeth.
- Injection Points: Typically 3 to 6 points per side (bilaterally), distributed across the belly of the muscle.
- Approach: Extraoral (from the outside of the face).
Temporalis Muscle
- Location: Fan-shaped muscle on the side of the head, above the zygomatic arch.
- Injection Points: Usually 2 to 4 per side.
- Approach: Extraoral.
Medial Pterygoid (Advanced Cases Only)
- Location: Lies deep inside the jaw near the back molars.
- Injection: Performed intraorally by experienced professionals.
- Use: Reserved for refractory or complex bruxism cases.
3. Typical Dosage Ranges
The dosage depends on several factors: muscle size, patient sensitivity, severity of symptoms, and formulation used. The following ranges are general guidelines for onabotulinumtoxinA (Botox®):
| Muscle | Units per Side | Total Bilateral Dose |
|---|---|---|
| Masseter | 20–30 units | 40–60 units |
| Temporalis | 10–20 units | 20–40 units |
| Medial Pterygoid | 10–15 units | 20–30 units |
Note: Dosing differs slightly for other formulations like Dysport or Xeomin due to potency variations. Always follow the manufacturer’s conversion recommendations.
Injection Summary Example (Moderate Bruxism Case):
Masseter (30 units per side) = 60 units
Temporalis (15 units per side) = 30 units
Total: 90 units of Botox
4. The Procedure: Step-by-Step
1. Preparation:
- The face is cleaned with antiseptic.
- Topical numbing cream may be applied, although the procedure is minimally painful.
- The patient is usually seated upright and asked to clench to help identify the masseter muscle borders.
2. Injection:
- A very fine needle (usually 30-gauge) is used.
- Botox is injected intramuscularly at pre-mapped locations.
- Each injection is small and takes only a few seconds.
3. Duration:
- The entire procedure typically takes 15 to 30 minutes.
- No sedation is required.
5. Post-Treatment Care and Follow-Up
After the procedure, patients can usually return to normal activities immediately. However, certain aftercare steps are recommended:
Post-Treatment Guidelines:
- Avoid lying flat or massaging the area for 4–6 hours.
- Refrain from strenuous physical activity for the rest of the day.
- Avoid excessive heat exposure (saunas, hot yoga) for 24 hours.
- Do not consume alcohol or blood-thinning medications (unless prescribed) immediately afterward, to reduce the risk of bruising.
Expected Effects:
- Onset: Noticeable symptom relief begins within 3 to 7 days.
- Peak Effect: 2 to 4 weeks post-injection.
- Duration: Effects typically last 3 to 6 months.
- Follow-Up: Most patients return for a reassessment and possible re-treatment every 4 to 6 months.
6. Adjusting the Dose Over Time
Botox therapy for bruxism is highly individualized. After the first treatment, the dosage may be adjusted upward or downward based on:
- Degree of symptom relief
- Muscle function during follow-up
- Any side effects (e.g., excessive muscle weakening)
- Aesthetic outcomes, such as reduction in jaw width
With regular monitoring, many patients achieve optimal relief with progressively lower doses over time, especially if behavioral or dental therapies are used in parallel.
Final Note on Administration
Botox for bruxism should only be administered by:
- Trained medical or dental professionals (MDs, DOs, DDS/DMDs) with expertise in facial anatomy.
- Clinicians familiar with both aesthetic and functional use of botulinum toxin.
Poor injection technique or dosing errors can lead to complications such as:
- Facial asymmetry
- Difficulty chewing
- TMJ instability
- Transient facial weakness
When performed correctly, however, the procedure is safe, effective, and well-tolerated by most patients.
Benefits of Botox for Bruxism Treatment
- Non-Invasive: Compared to surgical interventions, botulinum toxin injections are minimally invasive.
- Symptom Relief: Many patients report significant reduction in pain, muscle tension, and bruxism episodes.
- Aesthetic Improvement: Reduction in masseter hypertrophy can lead to a softer jawline, which may be desirable for some patients.
- Preventive Care: By decreasing grinding intensity, botulinum toxin can help prevent further dental wear and damage.
Potential Side Effects and Considerations
While generally considered safe, botulinum toxin treatment can have potential side effects:
- Muscle Weakness: Over-relaxation of the injected muscles can lead to difficulties in chewing or speaking.
- Asymmetry: Improper injection technique may result in facial asymmetry.
- Bruising or Pain at Injection Site: Common but typically transient.
- Headaches: Some patients may experience headaches post-treatment.
It’s crucial for patients to discuss their medical history and potential risks with their healthcare provider before undergoing treatment.
Frequently Asked Questions (FAQs)
Does Botox really work for bruxism?
Yes, Botox can be an effective treatment for bruxism, which involves chronic teeth grinding or jaw clenching—often during sleep or times of stress. Botox works by relaxing the masseter muscles, which are responsible for clenching. This reduces the intensity of the grinding and alleviates associated symptoms such as jaw pain, tension headaches, earaches, and even tooth damage. Many patients notice significant relief within a week or two of treatment, with full effects typically visible in about 2–4 weeks.
How long does Botox for bruxism last?
The effects of Botox for bruxism usually last between 3 to 6 months. The duration can vary depending on individual muscle activity, metabolism, and the amount of Botox used. Over time, with regular treatments, the masseter muscles may shrink slightly in size, leading to longer-lasting relief. Many people choose to repeat treatment every 4–5 months to maintain the benefits and prevent symptoms from returning.
How much does Botox for jaw clenching cost?
The cost of jaw Botox treatment can vary based on clinic location, practitioner expertise, and the amount of product required. In the UK, a typical session ranges between £200 and £500. Some clinics charge based on the number of units used, while others offer a flat rate per treatment area. It’s important to choose a qualified medical practitioner for the best and safest results.
What is the downside of Botox for TMJ?
While generally safe when administered by a qualified professional, Botox is not without risks. Potential side effects include temporary muscle weakness, bruising, swelling at the injection site, headaches, or a feeling of tightness in the jaw. In rare cases, over-relaxation of the jaw muscle can affect chewing or lead to asymmetry. Botox also doesn’t cure the underlying causes of TMJ or bruxism; it manages symptoms, meaning regular treatments are needed to maintain results.
Does Botox for bruxism change face shape?
Yes, one of the added benefits of Botox in the masseter area is that it can subtly slim and contour the lower face. Overactive masseter muscles can give the face a square or bulky jawline. When Botox relaxes these muscles, they gradually reduce in size due to decreased activity, leading to a softer, more V-shaped or oval facial appearance. This facial slimming effect usually becomes noticeable after a few weeks and is especially popular among those looking for a non-surgical jawline refinement.
Who is a good candidate for jaw Botox?
Ideal candidates for jaw Botox are individuals experiencing chronic jaw tension, teeth grinding, or clenching—especially if these issues haven’t responded to other treatments like night guards, physical therapy, or stress reduction. People seeking jaw slimming or facial contouring may also benefit. Candidates should be in good overall health, not pregnant or breastfeeding, and have realistic expectations about the results.
Does jaw Botox give you jowls?
Jaw Botox doesn’t directly cause jowls, but in rare cases, excessive reduction in muscle volume can contribute to skin sagging—especially in individuals with already loose or mature skin. When the masseter muscle reduces in size, the overlying skin may not adapt as quickly, leading to a loss of firmness. This is why it’s important to have the treatment done gradually and by an experienced injector who will consider your skin type, age, and facial structure.
