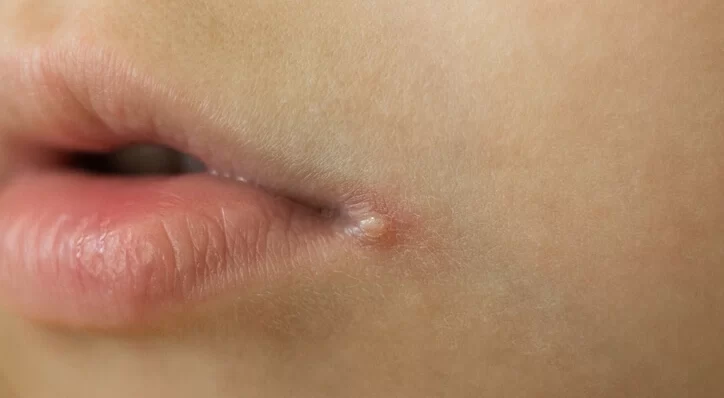
Angular cheilitis, also known as perleche or angular stomatitis, is a common condition characterized by inflammation, redness, fissures, and cracking at the corners of the mouth. This discomforting condition can be bothersome, impacting one’s ability to eat, speak, and smile comfortably. Understanding its causes, symptoms, available treatments, and preventive measures is crucial for managing and alleviating its effects.
Table of Contents
ToggleCauses of Angular Cheilitis
The exact cause of angular cheilitis can be multifactorial, often involving a combination of various factors:
- Fungal or Bacterial Infections
- Moisture and Saliva
- Nutritional Deficiencies
- Denture Use
- Skin Conditions
Fungal or Bacterial Infections
Candida albicans (yeast) and bacterial species like Staphylococcus aureus are commonly associated with angular cheilitis.
Moisture and Saliva
Excessive saliva accumulation at the corners of the mouth due to drooling, lip-licking, or ill-fitting dentures creates a favorable environment for fungal or bacterial growth.
Nutritional Deficiencies
Deficiencies in vitamins like B vitamins (especially B2, B3, B6, and B12), iron, and zinc can weaken the immune system and contribute to angular cheilitis.
Denture Use
Poorly fitting dentures can cause skin irritation and trapping of moisture, leading to angular stomatitis.
Skin Conditions
Eczema, psoriasis, or other skin conditions can predispose individuals to angular cheilitis due to compromised skin integrity.
Symptoms
The most prominent symptoms of angular cheilitis include:
- Pain, tenderness, or soreness at the corners of the mouth
- Redness, inflammation, or swelling
- Cracks, fissures, or splits in the skin, sometimes accompanied by bleeding
- Dryness or itching
- Formation of crusts or sores
Treatments for Angular Cheilitis
Treatment for angular cheilitis largely depends on the underlying cause. Here are various approaches that can be effective:
- Antifungal or Antibacterial Creams
- Topical Corticosteroids
- Vitamin and Mineral Supplements
- Moisturizers and Barrier Creams
- Denture Adjustment
Antifungal or Antibacterial Creams
Topical antifungal or antibacterial creams or ointments, such as clotrimazole or miconazole, can help clear up fungal or bacterial infections.
Topical Corticosteroids
These can be prescribed to reduce inflammation and promote healing, especially in cases associated with skin conditions like eczema.
Vitamin and Mineral Supplements
Supplementing with B vitamins, iron, and zinc can help if deficiencies are contributing to the condition.
Moisturizers and Barrier Creams
Applying petroleum jelly, beeswax, or other emollients can help protect the skin and prevent moisture accumulation.
Denture Adjustment
Ensuring well-fitted dentures or seeking dental assistance for adjustments can prevent irritation and moisture accumulation.
Preventive Measures
Taking preventive measures can significantly reduce the risk of developing angular cheilitis:
- Hygiene
- Nutrition
- Dental Care
- Stay Hydrated
- Avoid Irritants
Hygiene
Keep the corners of the mouth clean and dry. Avoid excessive licking of lips.
Nutrition
Maintain a balanced diet rich in vitamins and minerals to support immune health.
Dental Care
Ensure proper oral hygiene and regular dental check-ups, especially if wearing dentures.
Stay Hydrated
Drink an adequate amount of water to prevent dehydration.
Avoid Irritants
Limit exposure to potential irritants like harsh lip products or toothpaste that may exacerbate the condition.
When to Seek Medical Advice
While mild cases of angular cheilitis can often be managed with home remedies, it’s essential to consult a healthcare professional if:
- The condition persists for more than a few days despite home treatment.
- There’s severe pain, swelling, or bleeding.
- The sores become infected or spread.
Risk Factors and Complications
Several factors can increase the likelihood of developing angular cheilitis:
- Age
- Denture Wearers
- Weakened Immune System
- Nutritional Deficiencies
- Climate and Weather
Age
Elderly individuals, due to changes in skin integrity and immune function, are more susceptible.
Denture Wearers
Ill-fitting dentures or poor oral hygiene can contribute to the condition.
Weakened Immune System
Conditions like HIV/AIDS, diabetes, or autoimmune disorders can increase vulnerability to infections, including angular cheilitis.
Nutritional Deficiencies
Poor diet or malabsorption disorders can lead to deficiencies, exacerbating the risk.
Climate and Weather
Cold, dry weather or excessive moisture can aggravate the condition.
If left untreated or in severe cases, angular cheilitis can lead to complications such as secondary bacterial infections, scarring, or persistent discomfort affecting eating and speaking.
Home Remedies and Care
In addition to medical treatments, certain home remedies and self-care practices can complement the management of angular cheilitis:
- Honey
- Aloe Vera
- Good Oral Hygiene
- Warm Compresses
Honey
Applying raw honey to the affected area can offer antimicrobial benefits and promote healing.
Aloe Vera
Aloe vera gel has soothing properties and can aid in reducing inflammation.
Good Oral Hygiene
Regularly brush teeth and gently clean around the mouth with a soft toothbrush to prevent bacterial buildup.
Warm Compresses
Applying a warm, damp cloth to the affected area can provide relief from discomfort.
Conclusion
Angular cheilitis, though not usually serious, can cause discomfort and affect daily activities. Understanding its causes, symptoms, treatments, and preventive measures is crucial for effective management. By maintaining good oral hygiene, addressing nutritional deficiencies, and seeking appropriate medical advice when needed, individuals can alleviate the discomfort associated with this condition and prevent its recurrence.