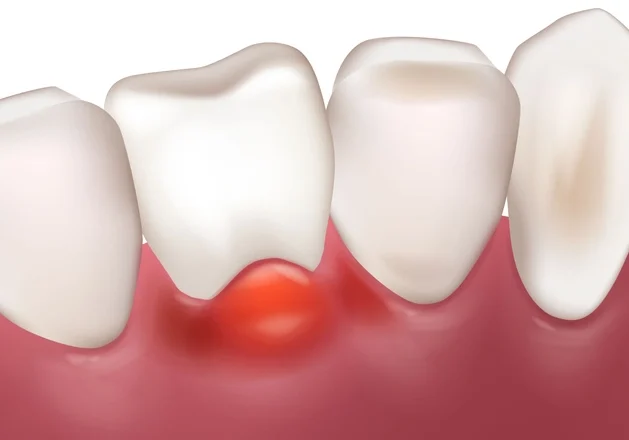
Periodontal abscesses represent a significant clinical challenge in dental practice, often presenting as painful swellings associated with periodontal pockets. They are localized purulent infections within the periodontal tissues and can arise suddenly, even in patients undergoing periodontal therapy. Despite being a common dental emergency, their pathophysiology, diagnosis, and management require a detailed understanding of periodontal anatomy, disease progression, and host immune responses.
Table of Contents
ToggleDefinition and Basic Concept
A periodontal abscess is defined as a localized collection of pus within the tissues of the periodontium adjacent to a periodontal pocket. It occurs as a result of bacterial invasion, leading to an acute inflammatory response characterized by tissue necrosis, exudate accumulation, and abscess cavity formation.
Unlike a periapical abscess, which originates from pulpal necrosis, a periodontal abscess arises from the supporting structures of the tooth — primarily the gingiva, periodontal ligament, and alveolar bone — and typically involves teeth with vital pulps. Understanding this distinction is fundamental for proper diagnosis and management.
Etiology and Pathogenesis
Introduction of Virulent Microorganisms
The most common initiating factor is the introduction of virulent organisms into a pre-existing periodontal pocket. Periodontal pockets, especially deep ones, provide a favorable anaerobic environment for bacteria such as Porphyromonas gingivalis, Prevotella intermedia, Fusobacterium nucleatum, and Aggregatibacter actinomycetemcomitans. These pathogens can invade the soft tissue wall of the pocket, triggering an acute inflammatory response that leads to pus formation.
Reduction in Drainage Potential
Another classic scenario for abscess formation occurs during periodontal treatment, particularly during scaling and root planing. As inflammation in the coronal gingiva subsides, the gingival margin becomes more tightly adapted to the tooth surface. This tighter adaptation can occlude the pocket entrance, blocking the drainage pathway for bacterial toxins and inflammatory exudate. The result is the accumulation of pus within the periodontal tissues, culminating in an abscess.
Foreign Body Impaction
The impaction of a foreign body, such as a fishbone, seed, or bristle from a toothbrush, can also precipitate a localized abscess. Such objects can penetrate the gingival sulcus or an existing pocket, introducing bacteria and causing mechanical irritation. Even in an otherwise healthy periodontal membrane, this can lead to abscess formation.
Opportunistic Superinfection
Patients who have recently received systemic antibiotic therapy for unrelated conditions may develop superinfections caused by opportunistic pathogens or resistant bacterial strains. When antibiotic coverage is incomplete or inappropriate, it may disrupt the normal oral microbiota and allow certain pathogens to flourish in untreated periodontal sites.
Underlying Systemic Factors
Patients with systemic conditions that impair immune response — such as uncontrolled diabetes mellitus, immunosuppressive therapy, HIV infection, or malnutrition — are predisposed to recurrent or multiple abscesses. The compromised immune defense allows for unchecked bacterial proliferation, and impaired healing exacerbates tissue breakdown.
Iatrogenic Causes
Certain dental procedures can inadvertently contribute to abscess formation. Improper scaling, incomplete debridement, or residual calculus left beneath the gingival margin can serve as persistent bacterial foci. Similarly, poorly adapted restorations that create plaque-retentive areas near gingival margins can lead to localized infection.
Pathophysiological Mechanism
The development of a periodontal abscess involves several stages:
- Bacterial invasion into the soft tissue wall of the periodontal pocket.
- Acute inflammatory response characterized by infiltration of neutrophils.
- Liquefaction necrosis of tissue due to bacterial enzymes and host-derived lysosomal enzymes.
- Pus accumulation within confined periodontal spaces.
- Increased pressure, leading to pain, swelling, and eventual sinus tract formation for drainage.
If left untreated, the infection can extend deeper, causing alveolar bone destruction and, in severe cases, spreading into fascial spaces leading to cellulitis.
Clinical Features
A periodontal abscess often presents acutely with pain and swelling localized to the affected area. The clinical manifestations include:
- Swelling of the gingiva, which may appear red, shiny, and edematous.
- Tenderness to palpation or percussion, often localized to the lateral aspect of the root.
- Pus discharge, which may be spontaneous or expressed through the gingival sulcus or sinus tract.
- Tooth mobility due to loss of periodontal attachment.
- Pain on lateral movements rather than vertical percussion.
- Possible systemic signs, including mild fever, malaise, and lymphadenopathy in severe cases.
Patients often describe a rapid onset of symptoms with a dull, throbbing pain that increases in intensity over hours or days.
Differential Diagnosis
The clinical picture of a periodontal abscess can resemble other orofacial infections. Therefore, establishing a precise diagnosis is crucial. The main conditions to differentiate include:
- Gingival Abscess
Localized to the gingival margin, often resulting from foreign body impaction without attachment loss. The tooth remains vital, and there is no involvement of the periodontal pocket. - Pericoronal Abscess
Associated with partially erupted teeth, especially mandibular third molars. The infection originates from the pericoronal flap (operculum). - Periapical Abscess
Originates from pulpal necrosis and is associated with non-vital teeth. Pain is usually elicited upon vertical percussion, and radiographs show periapical radiolucency and loss of lamina dura. - Combined Periodontal–Endodontic Lesion
This complex lesion involves both pulpal and periodontal pathology. Vitality testing and radiographic evaluation are essential to determine the primary source. - Other Lesions
Conditions such as cysts or neoplasms may mimic abscesses but usually present with chronic, non-tender swelling and different radiographic features.
Radiographic Findings
Radiographic examination may reveal:
- Vertical bone loss along the root surface.
- Loss of alveolar crest height.
- Intact lamina dura around the apex (distinguishing from periapical abscess).
- Occasionally, a lateral radiolucency corresponding to the abscess site.
Comparison Between Periapical and Periodontal Abscesses
| Feature | Periapical Abscess | Periodontal Abscess |
|---|---|---|
| Vitality | Non-vital tooth | Usually vital |
| Pain | Tender to vertical percussion | Pain on lateral movements |
| Mobility | May be mobile | Usually mobile |
| Radiographic Finding | Loss of lamina dura around apex | Loss of alveolar crest along root surface |
| Pocket Depth | Normal | Deep pocket present |
| Source of Infection | Pulpal necrosis | Periodontal pocket |
| Pus Discharge | Often through apex | Through gingival sulcus or sinus tract |
Diagnostic Aids
- Pulp Vitality Testing
Determines if the pulp is vital or non-vital, helping to distinguish periodontal from periapical abscesses. - Periodontal Probing
Reveals deep periodontal pockets in affected areas, often with pus discharge on pressure. - Radiographs
Periapical or bitewing radiographs help identify bone loss patterns. - Insertion of Gutta-Percha Point
In cases with sinus tracts, inserting a gutta-percha point followed by radiography can help trace the origin of infection. - Systemic Evaluation
In recurrent abscesses, evaluation for systemic diseases like diabetes is essential.
Emergency Management (Emergency Rx)
Immediate management focuses on relieving pain, reducing infection, and establishing drainage.
1. Drainage of Abscess
- Incision and Drainage under Local Anesthesia:
A small incision is made over the fluctuant area to allow pus to escape. This provides rapid symptom relief and prevents further spread of infection. - Drainage through the Pocket:
If the abscess is accessible through the periodontal pocket, gentle scaling and curettage can facilitate drainage.
2. Systemic Antibiotics
Antibiotics are indicated when there are systemic symptoms such as fever or lymphadenopathy. Common regimens include:
- Metronidazole: 200–400 mg three times daily for 5 days.
- Amoxicillin: 250–500 mg three times daily for 5 days.
In penicillin-allergic patients, alternatives like doxycycline or clindamycin may be prescribed.
3. Pain Management
Analgesics such as ibuprofen (400 mg every 6 hours) or paracetamol can help alleviate discomfort during the acute phase.
Further Management
Once the acute infection subsides and the patient is comfortable, attention must shift to eliminating the underlying cause.
1. Mechanical Debridement
Thorough scaling and root planing are performed to remove plaque, calculus, and necrotic tissue. Ultrasonic scalers and hand instruments may be used cautiously to prevent iatrogenic trauma.
2. Correction of Contributing Factors
- Removal of foreign bodies.
- Adjustment of overhanging restorations.
- Occlusal adjustment if traumatic occlusion is present.
3. Evaluation of Periodontal Status
Assess overall periodontal health, pocket depths, bone levels, and oral hygiene practices. Persistent deep pockets may require surgical intervention.
Follow-Up and Long-Term Care
1. Re-evaluation
After 1–2 weeks, the treated area should be re-examined for resolution of symptoms, reduction of pocket depth, and improvement in tissue tone.
2. Conventional Periodontal Therapy
Standard treatment for chronic periodontitis is implemented, including:
- Subgingival debridement.
- Plaque control education.
- Regular maintenance appointments.
3. Management of Combined Lesions
If an endodontic component is identified, appropriate root canal treatment must be performed before periodontal therapy to ensure complete resolution.
4. Surgical Management
In cases where the pocket remains deep or the abscess recurs, surgical procedures such as flap surgery, osseous recontouring, or regenerative therapy may be indicated.
Complications
If left untreated or improperly managed, periodontal abscesses can lead to severe consequences:
- Tooth loss due to extensive periodontal destruction.
- Spread of infection into fascial spaces, leading to cellulitis or Ludwig’s angina.
- Systemic infection in immunocompromised individuals.
- Chronic sinus tract formation, leading to intermittent drainage.
Prognosis
The prognosis depends on several factors:
- Extent of periodontal destruction prior to abscess formation.
- Promptness of treatment.
- Control of systemic risk factors (especially diabetes).
- Effectiveness of oral hygiene practices.
With timely intervention and proper maintenance, the prognosis can be favorable. However, in teeth with advanced attachment loss, extraction may be the only viable option.
Preventive Strategies
Preventing periodontal abscesses relies on maintaining good periodontal health and minimizing predisposing factors:
- Effective Oral Hygiene:
Regular brushing, flossing, and use of interdental cleaners prevent plaque accumulation. - Professional Maintenance:
Routine dental visits for scaling and polishing help control subgingival plaque and calculus. - Proper Periodontal Therapy:
Adequate post-treatment care after scaling and root planing ensures continued drainage and tissue healing. - Systemic Disease Control:
Patients with diabetes or immunodeficiency should maintain optimal medical control to enhance resistance against infection. - Patient Education:
Informing patients about the early signs of periodontal abscess, such as localized swelling or tenderness, encourages early dental consultation.
Conclusion
The periodontal abscess is a clinically significant condition that underscores the intimate relationship between microbial biofilm, host immune response, and systemic health. It serves as both a localized infection and a potential indicator of broader periodontal instability or systemic compromise.
Successful management requires not only immediate control of infection through drainage and antibiotics but also long-term strategies focused on the elimination of etiological factors and reinforcement of periodontal health. By understanding the distinct pathophysiological mechanisms, diagnostic features, and therapeutic principles, dental professionals can provide effective and comprehensive care to patients presenting with this common yet complex periodontal emergency.
References
- Lindhe, J., Lang, N. P., & Karring, T. (2015). Clinical Periodontology and Implant Dentistry (6th ed.). Wiley-Blackwell.
→ A comprehensive reference covering pathogenesis, diagnosis, and treatment of periodontal abscesses. - Newman, M. G., Takei, H., Klokkevold, P. R., & Carranza, F. A. (2019). Carranza’s Clinical Periodontology (13th ed.). Elsevier.
→ The standard textbook for understanding clinical manifestations and management of periodontal diseases. - Wilson, T. G., & Kornman, K. S. (1997). Fundamentals of Periodontics (2nd ed.). Quintessence Publishing Co.
→ Offers insight into microbiology and pathophysiology relevant to periodontal abscess formation. - Herrera, D., Roldán, S., & Sanz, M. (2000). The periodontal abscess: A review. Journal of Clinical Periodontology, 27(6), 377–386.
→ A landmark review summarizing clinical features, microbiology, and modern treatment approaches. - Herrera, D., Roldán, S., González, I., Sanz, M. (2002). The treatment of periodontal abscesses: A clinical study. Journal of Clinical Periodontology, 27(6), 377–386.
→ Provides empirical evidence for antibiotic selection and mechanical debridement outcomes. - American Academy of Periodontology. (2003). Parameter on acute periodontal diseases (including abscesses). Journal of Periodontology, 74(11 Suppl), 1848–1854.
→ Official practice parameters defining diagnostic and therapeutic standards. - Sanz, M., & Teughels, W. (2018). Innovations in nonsurgical periodontal therapy: Consensus report of the Sixth European Workshop on Periodontology. Journal of Clinical Periodontology, 45(Suppl 20), S3–S12.
→ Discusses modern debridement and adjunctive antibiotic protocols. - Slots, J., & Listgarten, M. A. (1988). Bacteroides gingivalis, Bacteroides intermedius, and Actinobacillus actinomycetemcomitans in human periodontal diseases. Journal of Clinical Periodontology, 15(2), 85–93.
→ Foundational research on microbial etiology in periodontal abscesses. - Haffajee, A. D., & Socransky, S. S. (1994). Microbial etiological agents of destructive periodontal diseases. Periodontology 2000, 5(1), 78–111.
→ In-depth discussion of bacterial complexes involved in abscess pathogenesis. - Flemmig, T. F. (1999). Periodontitis. Annals of Periodontology, 4(1), 32–38.
→ Offers context on disease progression leading to abscess formation. - Pihlstrom, B. L., Michalowicz, B. S., & Johnson, N. W. (2005). Periodontal diseases. The Lancet, 366(9499), 1809–1820.
→ A general review connecting systemic health and periodontal infections. - American Dental Association (ADA). (2020). Antibiotic Use in Dentistry: Evidence-Based Clinical Practice Guidelines.
→ Provides guidance on antibiotic stewardship in acute dental infections. - Albandar, J. M., & Rams, T. E. (2002). Global epidemiology of periodontal diseases: An overview. Periodontology 2000, 29(1), 7–10.
→ Background on the prevalence and risk factors related to abscess occurrence. - Keestra, J. A. J., Grosjean, I., Coucke, W., Quirynen, M., & Teughels, W. (2015). Non-surgical periodontal therapy with systemic antibiotics in patients with untreated chronic periodontitis: A systematic review and meta-analysis. Journal of Periodontal Research, 50(3), 294–314.
→ Evidence-based perspective on systemic antibiotic use in acute periodontal infections. - Jepsen, S., Caton, J. G., Albandar, J. M., et al. (2018). Periodontal manifestations of systemic diseases and developmental and acquired conditions: Consensus report of workgroup 3 of the 2017 World Workshop. Journal of Clinical Periodontology, 45(Suppl 20), S219–S229.
→ Discusses systemic links and immunocompromise in recurrent abscesses.