Periodontal diseases are among the most prevalent oral health conditions worldwide, characterized by inflammation and destruction of the supporting tissues of the teeth — the gingiva, periodontal ligament, cementum, and alveolar bone. Early diagnosis and continuous monitoring are vital for effective prevention, management, and prognosis. A comprehensive periodontal evaluation encompasses a thorough history, clinical and radiographic examination, and special investigations. The diagnostic process not only identifies the presence and extent of the disease but also determines contributing etiologic and risk factors that influence treatment planning and outcomes.
Table of Contents
ToggleHistory Taking
The first step in periodontal diagnosis is obtaining a detailed and systematic history. This process allows the clinician to understand the patient’s chief complaint, assess disease progression, and identify underlying risk factors.
Chief Complaint and Present Illness
Patients often report symptoms such as bleeding gums, halitosis, mobility of teeth, drifting of teeth, gingival recession, sensitivity, or the presence of abscesses. The clinician must establish the onset, duration, and pattern of symptoms — whether the condition is localized or generalized, intermittent or persistent, painful or asymptomatic.
For example, bleeding gums that occur only during brushing suggest superficial gingivitis, while spontaneous bleeding indicates deeper inflammation. Similarly, tooth mobility may reflect either acute inflammation or chronic bone loss.
Past Dental and Medical History
The patient’s previous dental treatments, oral hygiene practices, and compliance with maintenance care must be documented. Past experiences with scaling, root planing, periodontal surgeries, or extractions due to periodontal causes provide insight into disease behavior and patient attitude toward treatment.
Medical history plays a crucial role since systemic conditions can influence periodontal health. Diabetes mellitus, especially if poorly controlled, predisposes to more severe and recurrent periodontitis. Cardiovascular diseases, autoimmune disorders, osteoporosis, and hormonal changes are also linked to periodontal breakdown. Furthermore, medications such as anticonvulsants, calcium channel blockers, and immunosuppressants may induce gingival overgrowth, complicating diagnosis.
Risk Factor Assessment
Lifestyle and environmental factors must be considered. Smoking is one of the strongest modifiable risk factors, leading to impaired healing, increased attachment loss, and reduced response to therapy. Stress, nutrition, and socioeconomic status may also influence disease susceptibility.
Clinical Examination
A systematic clinical examination provides the foundation for diagnosis. It involves inspection, palpation, probing, and evaluation of both hard and soft tissues.
Plaque and Calculus Evaluation
Effective plaque control is essential for periodontal stability. The Plaque Index (PI) quantifies the presence of biofilm on four surfaces of each tooth (mesial, distal, buccal, and lingual). Disclosing agents can highlight plaque for both clinician and patient education. The index is expressed as a percentage of clean surfaces, which helps in setting measurable oral hygiene goals.
Supra- and subgingival calculus are detected by visual inspection and tactile exploration with a periodontal probe or explorer. Their removal during non-surgical therapy is fundamental for disease control.
Gingival Assessment
The gingiva should be examined for color, contour, consistency, and texture. In health, it is coral pink, firm, and stippled. Signs of inflammation include redness, swelling, loss of stippling, and bleeding upon gentle probing. The Marginal Bleeding Index (MBI) is a sensitive indicator of inflammation and patient oral hygiene compliance. It is calculated by gently running a probe around the sulcus and recording bleeding incidence as a percentage of total sites examined.
Periodontal Pocketing
The formation of periodontal pockets is the hallmark of periodontitis. A periodontal pocket is a pathologically deepened gingival sulcus resulting from apical migration of the junctional epithelium and loss of connective tissue attachment.
Types of Pockets:
1. False (Pseudo) Pockets:
Caused by gingival enlargement without attachment loss. The epithelial attachment remains at the cementoenamel junction (CEJ), and the increase in depth is due to coronal expansion of the gingiva.
2. True Pockets:
Involve actual loss of attachment, where the junctional epithelium migrates apically beyond the CEJ.
- Suprabony Pocket: The base of the pocket is coronal to the alveolar bone.
- Infrabony Pocket: The base of the pocket is apical to the alveolar crest.
Bone Defect Classification:
Infrabony defects are categorized based on the number of remaining bony walls:
- Three-walled defect: Surrounded by bone on three sides; favorable for regeneration.
- Two-walled defect: Typically a crater-shaped defect between adjacent teeth.
- One-walled defect: Least favorable for regeneration; open to soft tissues.
- Combined defect: A mix of the above configurations within the same site.
Periodontal Probing
Probing Pocket Depth (PPD)
Probing depth is measured from the gingival margin to the base of the pocket. It reflects current inflammatory status rather than the true historical loss of attachment.
However, in the presence of gingival enlargement, probing depth may overestimate the severity of attachment loss, while in cases of gingival recession, it may underestimate it.
Clinical Attachment Level (CAL)
The Clinical Attachment Level provides a more accurate measure of periodontal destruction, as it is measured from a fixed point—the cementoenamel junction—to the base of the pocket.
CAL = Pocket Depth + Recession (if present).
This measure allows comparison between visits and is essential for monitoring disease progression or healing following therapy.
Probes and Technique
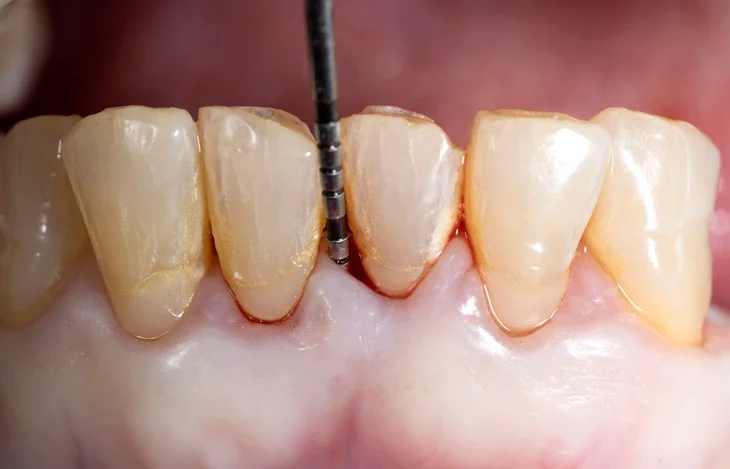
A periodontal probe is the principal instrument for detecting pockets. The WHO probe, used for the Basic Periodontal Examination (BPE), has a 0.5mm ball tip and a black band between 3.5mm and 5.5mm to aid visualization.
Probing Variables:
- Tissue Tone: Edematous tissues allow deeper penetration.
- Force Applied: Should be approximately 20–25g to prevent trauma.
- Probe Design: Diameter and calibration markings affect readings.
Inflamed tissue offers less resistance, and probes may penetrate beyond the junctional epithelium, leading to overestimation. Therefore, the term probing pocket depth is preferred to simply pocket depth.
Mobility Assessment
Tooth mobility is assessed using the handles of two instruments or fingers:
- Grade I: Slight mobility, <1mm horizontally.
- Grade II: Moderate mobility, >1mm horizontal but no vertical movement.
- Grade III: Severe mobility, with vertical displacement possible.
Increased mobility can result from attachment loss, trauma from occlusion, or inflammation of the periodontal ligament. It is important to distinguish between reversible (inflammatory) and irreversible (structural) causes.
Basic Periodontal Examination (BPE)
The BPE provides a rapid screening method to determine the need for further periodontal assessment.
- Codes 0–2: Indicate gingivitis or localized plaque/calculus issues manageable with improved hygiene.
- *Codes 3–4 and : Suggest periodontitis requiring full charting, detailed assessment, and possibly radiographs.
The mouth is divided into sextants, and the highest score in each sextant is recorded. This index is essential for risk assessment and treatment planning.
Radiographic Examination
Radiographs play a critical role in confirming clinical findings, assessing bone loss, and monitoring changes over time.
Indications
Radiographs are indicated for:
- Confirming diagnosis in patients with high BPE scores (3, 4, or *).
- Monitoring bone level stability during maintenance.
- Evaluating furcation involvement and periapical pathology.
- Investigating localized bone loss or angular defects.
Radiographic Techniques
- Bitewing Radiographs: Ideal for horizontal bone loss and interproximal calculus. Vertical bitewings are preferred when bone loss exceeds 5mm.
- Periapical Radiographs: Using the long cone paralleling technique, these provide detailed views of root morphology, periapical status, and vertical bone loss.
- Panoramic Radiographs (OPT): Useful for generalized assessment or when intraoral imaging is impractical, though they lack fine detail for precise measurements.
Interpretation
Bone loss is measured as a percentage of root length relative to the CEJ. The pattern of bone loss (horizontal vs. vertical) and presence of furcation defects should be recorded. Sequential radiographs taken with standardized angulation are invaluable for tracking disease progression or healing.
Record Keeping
Findings should be documented, including:
- Bone loss percentage and pattern.
- Presence of furcation involvement.
- Subgingival deposits.
- Any other pathology.
Diagnosis
Diagnosis integrates findings from history, clinical, and radiographic assessments. According to contemporary classification systems (2017 World Workshop), periodontal diseases are categorized based on stage (severity and complexity) and grade (rate of progression and risk factors).
For instance:
- Stage III, Grade B generalized periodontitis may be diagnosed in a smoker with 30–50% bone loss and moderate tooth mobility.
- Localized attachment loss without systemic risk factors may be classified as Stage II, Grade A.
This comprehensive framework helps clinicians plan appropriate interventions and communicate effectively across disciplines.
Monitoring and Disease Progression
Monitoring is the continuous evaluation of periodontal status over time to assess treatment outcomes and detect recurrence.
Clinical Monitoring
Key parameters include:
- Probing Pocket Depths (PPD) and CAL comparisons between visits.
- Bleeding on Probing (BOP): A sensitive indicator of inflammation and disease activity. Persistent bleeding at specific sites suggests active disease.
- Plaque and Bleeding Indices: Help gauge oral hygiene efficacy and patient compliance.
- Mobility and Furcation Changes: Reflect mechanical stability and treatment response.
Radiographic Monitoring
Sequential radiographs taken at 12- to 24-month intervals reveal bone level changes. Standardized positioning is crucial for accuracy.
Microbiological and Immunological Markers
Advanced diagnostic methods aim to detect pathogens (e.g., Porphyromonas gingivalis, Tannerella forsythia) and host response markers in gingival crevicular fluid. While promising for research, these tests are yet to achieve sufficient predictive accuracy for routine clinical use.
Summary of Diagnostic and Monitoring Principles
- Comprehensive History:
Include medical, dental, and social factors to identify systemic influences. - Clinical Examination:
Evaluate gingiva, plaque, calculus, probing depths, and mobility. - BPE Screening:
Use as an initial tool to determine the need for full periodontal charting. - Radiographic Assessment:
Employ bitewings and periapicals judiciously to confirm bone loss patterns. - Diagnosis and Classification:
Apply the latest staging and grading system for standardized reporting. - Monitoring:
Record and compare data across appointments to detect disease progression or remission. - Patient Education:
Reinforce plaque control, smoking cessation, and maintenance visits as essential to long-term stability.
The Role of Bleeding on Probing (BOP)
Bleeding on probing remains one of the most reliable clinical indicators of periodontal inflammation. The absence of BOP is strongly associated with stability, whereas its presence suggests active disease. However, it should not be used in isolation — rather, as part of a comprehensive assessment including probing depths, attachment levels, and radiographs.
Advancements in Periodontal Diagnostics
Recent research has focused on improving diagnostic precision through:
- Digital Probing Devices: Automated force-controlled probes increase reproducibility.
- 3D Imaging (CBCT): Allows detailed visualization of bone morphology and defects.
- Biomarker Analysis: Detection of inflammatory mediators like interleukin-1β and matrix metalloproteinases in saliva and GCF may enhance early detection of active disease.
These innovations aim to supplement traditional methods rather than replace them, offering greater insight into disease mechanisms and risk prediction.
Conclusion
Accurate diagnosis and diligent monitoring are the cornerstones of successful periodontal care. A structured approach beginning with comprehensive history taking, followed by meticulous clinical and radiographic evaluation, allows for precise disease classification and effective management planning. Continuous monitoring through probing, bleeding assessment, and radiographs ensures timely intervention and long-term stability.
Ultimately, the clinician’s skill in synthesizing diagnostic data, coupled with patient education and compliance, determines the prognosis. As diagnostic technologies evolve, combining classical clinical methods with modern adjunctive tools promises even greater accuracy and individualized care in the future of periodontology.
References
- Lang NP, Bartold PM. Periodontal health. J Clin Periodontol. 2018;45(Suppl 20):S9–S16.
- Chapple ILC, Mealey BL, Van Dyke TE, et al. Periodontal health and gingival diseases and conditions on an intact and a reduced periodontium: Consensus report of workgroup 1 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J Clin Periodontol. 2018;45(Suppl 20):S68–S77.
- Tonetti MS, Greenwell H, Kornman KS. Staging and grading of periodontitis: Framework and proposal of a new classification and case definition. J Periodontol. 2018;89(Suppl 1):S159–S172.
- Lindhe J, Lang NP, Karring T. Clinical Periodontology and Implant Dentistry. 6th ed. Oxford: Wiley-Blackwell; 2015.
- Carranza FA, Newman MG. Carranza’s Clinical Periodontology. 13th ed. Philadelphia: Elsevier Saunders; 2019.
- Listgarten MA. Periodontal probing: What does it mean? J Clin Periodontol. 1980;7(3):165–176.
- Lang N, Adler R, Joss A, Nyman S. Absence of bleeding on probing: An indicator of periodontal stability. J Clin Periodontol. 1986;13(6):590–596.
- Armitage GC. Development of a classification system for periodontal diseases and conditions. Ann Periodontol. 1999;4(1):1–6.
- American Academy of Periodontology (AAP). Comprehensive periodontal evaluation: Parameters of care. J Periodontol. 2015;86(7 Suppl):S1–S23.
- Pihlstrom BL, Michalowicz BS, Johnson NW. Periodontal diseases. Lancet. 2005;366(9499):1809–1820.
- Lang NP, Tonetti MS. Periodontal risk assessment (PRA) for patients in supportive periodontal therapy (SPT). Oral Health Prev Dent. 2003;1(1):7–16.
- Loos BG, Van Dyke TE. The role of inflammation and genetics in periodontal disease. Periodontol 2000. 2020;83(1):26–39.
- Jepsen S, Caton JG, Albandar JM, et al. Periodontal manifestations of systemic diseases and developmental and acquired conditions: Consensus report. J Clin Periodontol. 2018;45(Suppl 20):S171–S189.
- Lang NP, Tonetti MS. Monitoring disease during supportive periodontal therapy. Periodontol 2000. 1996;12(1):91–100.
- Kinane DF, Stathopoulou PG, Papapanou PN. Periodontal diseases. Nat Rev Dis Primers. 2017;3:17038.