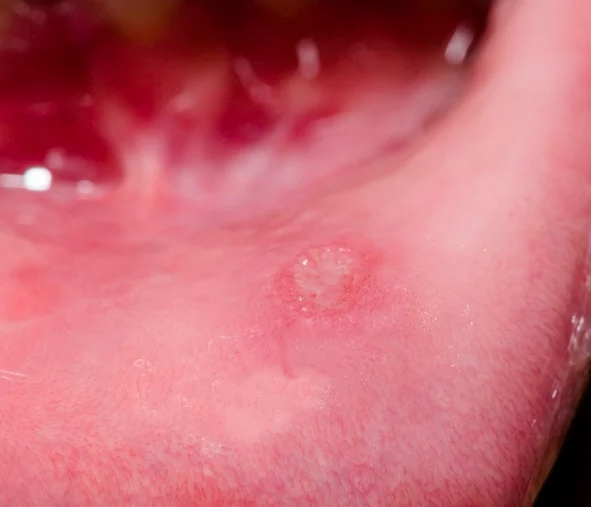
Vesiculo-bullous lesions of the oral cavity represent a heterogeneous group of disorders characterized by the formation of vesicles (small fluid-filled blisters) or bullae (larger blisters). These lesions arise due to separation within or beneath the epithelial layers of the oral mucosa. Based on the level of tissue cleavage, vesiculo-bullous diseases are broadly classified into intraepithelial and subepithelial lesions.
This article focuses on subepithelial vesiculo-bullous lesions, in which the separation occurs at the epithelium–connective tissue junction or below the basement membrane. Because the epithelium remains intact, the bullae in these conditions tend to be tense and firm, unlike intraepithelial bullae which rupture easily. Subepithelial vesiculo-bullous disorders often have autoimmune, genetic, or hypersensitivity-related etiologies and can involve both oral and extra-oral tissues.
Understanding these conditions is essential for dental and medical professionals, as oral manifestations may be the first or only sign of systemic disease, and early recognition can prevent severe complications such as scarring, blindness, infection, or malignancy.
Table of Contents
TogglePathophysiology of Subepithelial Bullae
The hallmark of subepithelial vesiculo-bullous disorders is disruption at the basement membrane zone (BMZ), which anchors the epithelium to underlying connective tissue. Damage may occur due to:
- Autoantibodies directed against basement membrane proteins
- Genetic defects in anchoring fibrils or collagen
- Immune complex deposition
- Hypersensitivity reactions
Because the epithelium remains structurally intact, the resulting bullae are less fragile, often blood-filled, and persist longer than intraepithelial blisters.
Angina Bullosa Haemorrhagica
Definition and Epidemiology
Angina bullosa haemorrhagica (ABH) is an acute, benign condition characterized by the sudden appearance of a blood-filled blister in the oral cavity. Despite its alarming presentation, it is not associated with systemic disease or hematological abnormalities. It occurs most commonly in elderly individuals.
Etiology and Pathogenesis
The exact etiology of ABH remains unknown. However, several predisposing factors have been proposed:
- Minor trauma during eating (sharp foods, hot drinks)
- Fragility of mucosal blood vessels
- Long-term use of inhaled corticosteroids
- Age-related mucosal atrophy
The lesion forms due to a break at the epithelium–connective tissue junction, leading to bleeding from superficial capillaries and subsequent bulla formation.
Clinical Features
- Sudden onset, often during meals
- Single, tense, dark red or purple blister
- Common sites: soft palate, lateral tongue, buccal mucosa
- Usually painless but may cause discomfort or choking sensation
- Rapid rupture within hours, followed by spontaneous healing without scarring
Diagnosis and Management
Diagnosis is clinical. It is essential to exclude serious bullous disorders such as pemphigus vulgaris and mucous membrane pemphigoid.
Management is conservative:
- Reassurance of the patient
- Sterile puncture if the blister interferes with speech or swallowing
- No specific drug therapy is required
Mucous Membrane Pemphigoid
Overview and Epidemiology
Mucous membrane pemphigoid (MMP) is a chronic autoimmune subepithelial blistering disease predominantly affecting mucous membranes. It occurs most commonly in women over 60 years of age.
Etiology and Immunopathogenesis
MMP is caused by autoantibodies (IgG and C3) directed against components of the basement membrane, including BP180 and BP230 antigens. These antibodies activate complement, leading to inflammation and separation of epithelium from connective tissue.
Clinical Features
Oral Manifestations
- Tense bullae that rupture to form painful erosions
- Desquamative gingivitis is a common presentation
- Lesions heal slowly and often with scarring
Extra-Oral Involvement
- Conjunctiva (ocular pemphigoid) → risk of blindness
- Nasal, pharyngeal, laryngeal, and genital mucosa
Because ocular scarring may be irreversible, oral signs are considered an important warning sign.
Diagnosis
- Histopathology: subepithelial split
- Direct immunofluorescence: linear deposition of IgG and C3 at basement membrane
- Indirect immunofluorescence may support diagnosis
Management
MMP requires long-term management:
- Mild disease: topical corticosteroids
- Moderate to severe disease: systemic steroids
- Steroid-sparing agents: azathioprine, methotrexate, dapsone
- Mandatory referral to ophthalmology
Despite its chronic nature, the prognosis is generally benign if managed appropriately.
Bullous Pemphigoid
Definition and Epidemiology
Bullous pemphigoid is a chronic autoimmune blistering disease primarily affecting the elderly (>60 years). It is more common than pemphigus vulgaris but less severe.
Pathogenesis
Autoantibodies (IgG) target proteins of the epithelial basement membrane, resulting in subepithelial blister formation.
Clinical Features
- Firm, tense bullae on skin
- Oral involvement occurs in only 20% of patients
- Bullae are less likely to rupture than in pemphigus
- Lesions heal without scarring
Bullous pemphigoid may occasionally act as a marker for internal malignancy or a drug-induced immune reaction.
Diagnosis and Treatment
Diagnosis involves biopsy and immunofluorescence.
Treatment includes:
- Topical or systemic corticosteroids
- Immunosuppressive therapy if severe
Prognosis is generally good compared to other autoimmune blistering disorders.
Dermatitis Herpetiformis
Overview
Dermatitis herpetiformis is a rare, chronic blistering disorder strongly associated with gluten sensitivity and celiac disease. It predominantly affects middle-aged men.
Pathogenesis
Autoantibodies against:
- Gliadin
- Endomysium
- Tissue transglutaminase
These antibodies lead to immune complex deposition in the skin and mucosa.
Clinical Features
- Intensely pruritic skin lesions
- Oral lesions present in ~70% of patients with skin involvement
- Bullae rupture to form large, painful erosions
- Both skin and mucous membranes are affected
Management
- Dapsone (diagnostic and therapeutic)
- Strict gluten-free diet
Early dietary control significantly improves prognosis.
Lichen Planus (Bullous Variant)
General Overview
Lichen planus is a chronic inflammatory disorder affecting skin and mucous membranes. The bullous variant is rare.
Clinical Features
- Subepithelial bullae that rupture easily
- Result in large erosions
- Often associated with reticular or erosive lichen planus
Management
Treatment focuses on:
- Topical or systemic corticosteroids
- Symptomatic relief
- Long-term follow-up due to malignant transformation risk in oral lichen planus
Epidermolysis Bullosa
Definition and Classification
Epidermolysis bullosa (EB) is a group of genetically inherited blistering disorders characterized by extreme fragility of skin and mucosa.
The dystrophic autosomal recessive form is most relevant to oral medicine.
Clinical Features
- Appears shortly after birth
- Bullae form after minor trauma
- Painful oral erosions
- Dental enamel hypoplasia
- High caries susceptibility
Healing occurs with scarring, leading to:
- Microstomia
- Ankyloglossia
- Dysphagia and speech difficulties
Complications
- Severe scarring
- Destruction of extremities
- Increased risk of squamous cell carcinoma
Management
- Supportive care
- Trauma avoidance
- Steroids and phenytoin may help in some forms
- Multidisciplinary management is essential
Erythema Multiforme
Definition
Erythema multiforme (EM) is an acute, immune-mediated hypersensitivity reaction affecting skin and mucous membranes, most commonly in young adult males.
Etiology
Triggers include:
- Drugs (penicillins, NSAIDs, carbamazepine)
- Infections (HSV, Mycoplasma pneumoniae)
- Sunlight
- Pregnancy
- Malignancy
- Chemical agents
Clinical Features
- Target lesions on skin
- Oral bullae in 70% of cases
- Crusted lips and painful erosions
- Fever and malaise
Disease Spectrum
- Minor EM: mild, self-limiting
- Major EM: severe mucosal involvement
- Stevens-Johnson syndrome
- Toxic epidermal necrolysis (TEN)
Management
- Identify and eliminate trigger
- Supportive care and hydration
- Chlorhexidine mouthwash
- Antivirals if HSV-related
- Severe cases: systemic steroids and azathioprine
Linear IgA Disease
Overview
Linear IgA disease is a rare autoimmune blistering disorder, often identified histologically.
Clinical Features
- Non-specific oral ulceration
- Rare bullae formation
Diagnosis and Management
- Direct immunofluorescence shows linear IgA deposition
- Treated with systemic steroids or mycophenolate mofetil
Conclusion
Subepithelial vesiculo-bullous lesions encompass a diverse group of disorders with overlapping clinical features but distinct etiologies, prognoses, and management strategies. Oral healthcare professionals play a vital role in early diagnosis, particularly because oral lesions may precede skin or systemic involvement.
A thorough understanding of these conditions—combined with careful clinical examination, histopathological assessment, and immunological testing—is essential for accurate diagnosis and effective management. Early recognition not only alleviates patient discomfort but can also prevent devastating complications such as blindness, severe scarring, or malignancy.