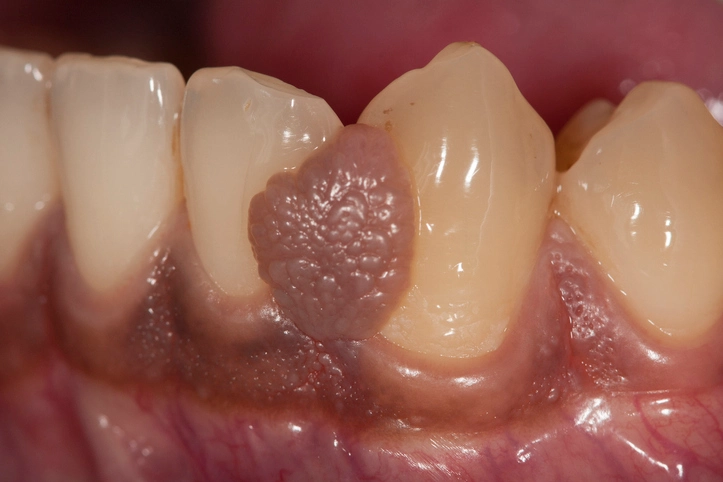
Pigmented lesions of the oral cavity represent a diverse group of conditions that vary widely in etiology, clinical appearance, biological behavior, and clinical significance. While pigmentation in the mouth may be alarming to patients and clinicians alike, many oral pigmented lesions are benign and harmless. Others, however, may represent systemic disease or, in rare cases, life-threatening malignancy. For this reason, understanding oral pigmentation is essential for accurate diagnosis, appropriate management, and timely referral when necessary.
The grouping of pigmented lesions of the oral mucosa is somewhat artificial, as these lesions are not unified by a single pathological mechanism or treatment approach. Instead, they encompass developmental, reactive, systemic, infectious, neoplastic, and iatrogenic processes. Despite this heterogeneity, pigmented oral lesions are a popular and important topic in clinical examinations, particularly in dentistry and oral medicine, because they test a clinician’s ability to recognize patterns, differentiate benign from malignant disease, and integrate oral findings with systemic health.
Clinically, one of the most useful frameworks for approaching oral pigmentation is to determine whether the pigmentation is localized or generalized. Localized lesions typically suggest focal pathology such as foreign body implantation, benign melanocytic proliferations, or neoplasia. Generalized pigmentation, by contrast, often reflects physiologic variation, systemic disease, or drug-related effects.
Table of Contents
ToggleBasic Principles of Oral Pigmentation
Pigmentation of the oral mucosa may result from several mechanisms:
- Melanin deposition – increased production or accumulation of melanin by melanocytes
- Exogenous pigments – foreign materials embedded in the mucosa
- Blood products – hemoglobin, hemosiderin, or other breakdown products
- Microbial pigments – produced by bacteria or fungi
- Chemical staining – from foods, drugs, or tobacco
The color of oral pigmentation can range from light brown to dark black, blue, purple, or even greenish hues, depending on the underlying cause and depth of pigment deposition. Superficial pigments tend to appear brown, whereas deeper pigments may appear blue or gray due to the Tyndall effect.
A careful clinical examination should always assess:
- Color
- Size
- Shape
- Borders
- Surface texture
- Location
- Duration
- Symptoms
- Change over time
These features, combined with patient history and risk factors, guide diagnosis and management.
Localized Pigmented Lesions
Localized pigmented lesions are confined to a specific area of the oral mucosa and often have identifiable local causes. While most are benign, localized pigmentation demands careful evaluation to exclude malignancy.
Amalgam Tattoo and Other Foreign Body Pigmentation
Etiology and Pathogenesis
An amalgam tattoo is the most common cause of localized blue-black pigmentation in the oral cavity. It occurs when dental amalgam particles become embedded in the oral mucosa. This may happen during:
- Placement or removal of amalgam restorations
- Tooth extraction near amalgam-restored teeth
- Fracture of amalgam fillings
Other foreign materials can cause similar lesions, including graphite from pencils or grit embedded following trauma, sometimes referred to as “road rash.”
Clinical Features
Amalgam tattoos typically present as:
- Flat or slightly raised lesions
- Blue, black, or gray in color
- Well-defined or diffuse borders
- Most commonly on the gingiva, buccal mucosa, or alveolar mucosa
They are usually asymptomatic and discovered incidentally during routine examination.
Diagnosis
Diagnosis is primarily clinical, supported by:
- History of dental restorations
- Characteristic appearance
- Radiographic evidence of radiopaque particles in some cases
If uncertainty exists, biopsy may be performed to exclude melanocytic lesions.
Management
Amalgam tattoos require no treatment if asymptomatic and confidently diagnosed. Patient reassurance is usually sufficient. Surgical removal may be considered for diagnostic uncertainty or aesthetic concerns.
Pigmentation Associated with Chronic Trauma
Etiology
Chronic mechanical irritation from:
- Sharp teeth
- Ill-fitting dentures
- Orthodontic appliances
- Habitual biting
can lead to reactive changes in the oral mucosa.
Clinical Features
These lesions usually present as areas of:
- Hyperkeratosis
- Leukoplakia-like thickening
- Occasionally brown or dark pigmentation
Pigmentation may occur secondary to post-inflammatory melanosis.
Management
Management focuses on eliminating the source of trauma. Lesions should be reviewed for resolution, and persistent pigmented lesions may warrant biopsy.
Ephelis (Oral Freckles)
Definition
Ephelides are small, benign, freckle-like lesions of the oral mucosa caused by localized increases in melanin deposition without an increase in melanocyte number.
Clinical Features
- Small, well-defined brown macules
- Common on lips and buccal mucosa
- Asymptomatic and stable over time
Clinical Significance
Ephelides are harmless and require no treatment. Differentiation from early melanocytic lesions is important, particularly if lesions change in size or color.
Pigmented Naevi of the Oral Mucosa
Overview
Oral pigmented naevi are rare benign proliferations of melanocytes, analogous to cutaneous moles.
Common Sites
- Vermilion border of the lips
- Hard palate
- Gingiva
Clinical Features
- Small (<1 cm)
- Well-circumscribed
- Brown, blue, or black
- Typically stable over time
Clinical Importance
Although benign, oral naevi warrant monitoring. Any lesion that enlarges, darkens, or becomes irregular should be biopsied to exclude melanoma.
Peutz–Jeghers Syndrome
Overview
Peutz–Jeghers syndrome is an inherited condition characterized by mucocutaneous pigmentation and gastrointestinal polyposis.
Oral Manifestations
- Multiple small brown or black macules
- Commonly around the lips and oral commissures
- May also involve buccal mucosa and tongue
Clinical Significance
While the pigmentation itself is benign, the syndrome carries a significant risk of gastrointestinal and extraintestinal malignancies. Recognition of oral pigmentation can prompt life-saving systemic investigation.
Kaposi’s Sarcoma
Etiology
Kaposi’s sarcoma is a vascular malignancy associated with human herpesvirus-8 infection and immunosuppression, particularly in individuals with HIV/AIDS.
Oral Features
- Red, purple, or brown macules, plaques, or nodules
- Commonly affects the palate and gingiva
- May ulcerate or bleed
Clinical Importance
Oral Kaposi’s sarcoma may be an early sign of underlying immunodeficiency. Management involves oncologic and medical treatment, often with good response to radiotherapy.
Oral Malignant Melanoma
Overview
Oral malignant melanoma is a rare but highly aggressive malignancy arising from melanocytes of the oral mucosa.
Clinical Features
- Very dark pigmentation
- Irregular borders
- Asymmetry
- Rapid enlargement
- Common sites: palate and maxillary gingiva
A rare variant may be non-pigmented, making diagnosis particularly challenging.
Prognosis and Management
Oral melanoma carries a poor prognosis due to late presentation and early metastasis. Early recognition, biopsy, and referral are critical.
Generalized Pigmented Lesions
Generalized pigmentation affects multiple areas of the oral mucosa and often reflects physiologic, systemic, or iatrogenic causes.
Racial (Physiologic) Pigmentation
Overview
Physiologic oral pigmentation varies with skin type and genetic background.
Clinical Features
- Diffuse brown pigmentation
- Common on gingiva, buccal mucosa, and palate
- Symmetrical and stable
Clinical Significance
This pigmentation is entirely benign and requires no treatment.
Pigmentation Due to Foodstuffs
Certain foods and habits can stain the oral mucosa.
Common Causes
- Tobacco
- Betel quid (paan)
- Strongly pigmented foods and beverages
Management
Improved oral hygiene and cessation of staining habits often lead to resolution.
Drug-Induced Oral Pigmentation
Several medications can cause oral mucosal pigmentation.
Common Offenders
- Antimalarials
- Phenothiazines
- Chemotherapeutic agents
- Oral contraceptives
- Chlorhexidine mouthwash (especially when combined with tea or tobacco)
Clinical Features
- Diffuse or patchy brown pigmentation
- May affect tongue, gingiva, or mucosa
Management
Pigmentation may resolve after discontinuation of the offending agent, though this is not always possible or necessary.
Heavy Metal Pigmentation
Etiology
Chronic exposure to heavy metals such as lead or mercury may cause pigmentation along the gingival margin.
Clinical Features
- Linear discoloration at gingival margins
- Rare in modern practice
Recognition is important as it may indicate systemic toxicity.
Endocrine-Associated Pigmentation
Addison’s Disease and Related Disorders
Increased adrenocorticotropic hormone (ACTH) levels stimulate melanocytes, resulting in pigmentation.
Oral Features
- Diffuse brown pigmentation
- Often affects buccal mucosa and gingiva
Systemic Signs
- Low blood pressure
- Fatigue
- Electrolyte imbalance
Oral findings may precede systemic diagnosis.
Haemochromatosis
Overview
Haemochromatosis causes iron overload with deposition of hemosiderin in tissues.
Oral Manifestations
- Generalized hyperpigmentation
- Rare oral involvement
Recognition may aid in early diagnosis of systemic disease.
Black Hairy Tongue
Pathogenesis
Black hairy tongue results from:
- Overgrowth of pigment-producing microorganisms
- Elongation of filiform papillae
- Reduced desquamation
Clinical Features
- Black, brown, or yellow discoloration of the tongue dorsum
- Hair-like appearance
- Often associated with poor oral hygiene, smoking, or antibiotics
Management
Reassurance, improved oral hygiene, and tongue scraping are usually effective.
Conclusion
Pigmented lesions of the oral cavity encompass a wide spectrum of conditions, ranging from harmless physiologic variations to aggressive malignancies. A structured approach based on localization, clinical appearance, patient history, and risk factors allows clinicians to differentiate benign from serious pathology effectively. Oral healthcare professionals play a critical role in identifying these lesions, reassuring patients when appropriate, and ensuring timely referral for potentially life-threatening conditions.
Understanding oral pigmentation is not merely an academic exercise—it is an essential component of comprehensive oral and systemic healthcare.