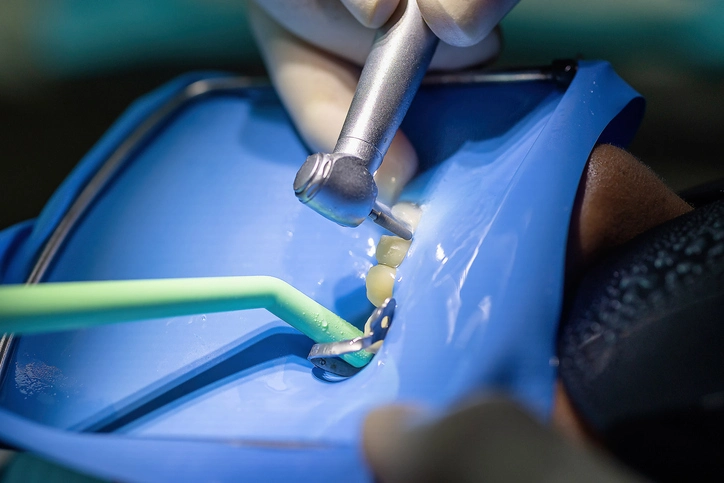
Isolation and moisture control are foundational principles in restorative dentistry, playing an essential role in ensuring the success and longevity of dental restorations. A controlled and moisture-free operating field is critical not only for optimal adhesion and restorative outcomes but also for patient safety and operator efficiency. The oral environment presents constant challenges to maintaining dryness due to the presence of saliva, gingival crevicular fluid, blood, and breath moisture. Therefore, effective isolation techniques are necessary to manage these sources of contamination while improving visibility, access, and patient comfort.
Table of Contents
ToggleThe Rationale for Isolation and Moisture Control
In dental restorative procedures, the ability to control moisture directly affects the integrity and strength of the final restoration. Modern adhesive systems and restorative materials, such as resin composites, glass ionomer cements, and bonding agents, are highly sensitive to contamination by saliva, blood, or moisture. Even minimal exposure to moisture during the bonding process can lead to decreased bond strength, microleakage, postoperative sensitivity, and premature failure of restorations.
Beyond material considerations, proper isolation also serves several additional purposes:
- Patient Safety: Prevents aspiration or ingestion of instruments, debris, and caustic materials.
- Operator Visibility: Ensures a clear, well-lit, and dry field for precision work.
- Infection Control: Reduces the spread of aerosols and contamination of instruments.
- Comfort and Efficiency: Decreases treatment time by preventing repeated interruptions to clear fluids from the operating site.
In essence, isolation and moisture control contribute not only to the technical success of restorative procedures but also to the broader principles of patient safety, ergonomics, and clinical quality assurance.
Aspiration and Evacuation Systems
A key element in moisture control involves the management of fluids using aspiration and suction systems. These are categorized based on the volume of fluid they can handle and the manner in which they are used.
High-Volume Suction
High-volume evacuation (HVE), often referred to as an aspirator, is designed to remove large quantities of water, debris, and saliva rapidly from the oral cavity. It is essential during procedures that generate aerosols, such as ultrasonic scaling or tooth preparation with rotary instruments. The HVE system not only maintains a clear field but also helps control the spread of infectious aerosols, thereby improving safety for both patient and clinician.
Effective use of high-volume suction requires proper angulation and placement of the suction tip. The assistant or operator should position it close to the working area but not in direct contact with tissues, to prevent trauma or obstruction of the clinician’s view. Specialized tips with ergonomic designs and autoclavable materials are available for different procedures.
Low-Volume Suction
Low-volume suction, typically achieved through a saliva ejector, is used to remove small amounts of saliva and fluid from the mouth. It is ideal for less invasive procedures or when high-volume suction is not required. While saliva ejectors are effective in maintaining general moisture control, they are not sufficient for aerosol management or heavy fluid evacuation. They should never be used to aspirate large volumes of fluid or debris, as this could result in blockage or cross-contamination.
Compressed Air
Compressed air is frequently employed to dry the operating field, enhance visibility, and ensure the surface is ready for bonding or restorative placement. However, compressed air tends to redistribute moisture rather than remove it entirely, which may lead to splattering or accidental contamination of nearby surfaces (including the clinician’s eyes). Prolonged use of air directly onto dentine can also cause desiccation and pulpal irritation. Therefore, air should be used cautiously, particularly in deep cavities or near vital tissues. Short, controlled bursts of air are recommended for safe drying.
Absorbents
Absorbent materials are passive aids that help to control moisture by physically soaking up saliva, crevicular fluid, or blood. They are particularly useful when suction alone is insufficient or impractical.
Cotton-Wool Rolls
Cotton-wool rolls are among the most common absorbent materials used in dentistry. They are inserted into the buccal and lingual vestibules, typically near the parotid and submandibular duct openings, to absorb saliva and maintain a dry field. The insertion should be performed using a rolling motion away from the alveolar ridge to avoid mucosal trauma. Before removal, the cotton rolls must be moistened to prevent adhesion to mucosa, which could lead to discomfort or tearing.
Paper Pads
Paper pads are disposable absorbents used in various areas of the oral cavity, especially under the tongue or cheeks. They help supplement suction systems during restorative procedures or prophylaxis.
Carboxymethylcellulose Pads (Dry Tips®)
These are advanced absorbent pads that adhere to the buccal mucosa and are designed to block the parotid duct. Their impermeable plastic backing prevents saliva from reaching the operative field. When inserted correctly—plastic side toward the tooth—they provide excellent isolation, particularly during posterior restorative or sealant procedures.
Rubber Dam Isolation
The rubber dam remains the gold standard for isolation in restorative dentistry. Its use creates a dry, aseptic field by physically separating the tooth or teeth under treatment from the rest of the oral cavity. Despite requiring some practice, it offers unmatched advantages in terms of visibility, moisture control, and patient protection.
Benefits of the Rubber Dam
- Eliminates Salivary Contamination: Completely isolates the operating field from saliva and blood.
- Improves Access and Visibility: Retracts soft tissues and prevents mirror fogging.
- Protects the Airway: Prevents aspiration or swallowing of instruments, debris, or chemicals.
- Enhances Bond Strength: Provides a clean, uncontaminated surface for adhesive procedures.
- Reduces Cross-Contamination: Acts as a barrier against aerosol and splatter spread.
For these reasons, the use of a rubber dam is mandatory in certain procedures, such as root canal therapy (RCT), where failure to use it is considered negligent due to patient safety risks.
Components of a Rubber Dam System
- Rubber Dam Sheet: Made of latex or non-latex material, available in various gauges and sizes.
- Clamps: Metal jaws that secure the dam around the tooth.
- Frame: Holds the dam taut and prevents obstruction.
- Punch and Forceps: Used to create holes and place clamps accurately.
- Floss Ligatures or Wedges: Used for additional stabilization.
Types of Rubber Dam
- Sheet Grade (6-inch square / 15 cm): Supported with a frame; moderate to thicker gauges are preferred for durability and retraction.
- Mask Type or ‘Dry Dam’: Supported by a paper frame, looped over the ears with elastic.
- Latex-Free Dams: Increasingly common to accommodate patients with latex allergies.
- OptraGate®: A lip and cheek retractor alternative that aids isolation without a full dam setup.
- OptiDam™: An anatomically shaped dam designed to fit more naturally around oral contours.
Securing the Rubber Dam
Several methods can be used to anchor the dam to the teeth:
- Rubber Dam Clamps: Metal clamps that grip the cervical portion of the tooth.
- Floss Ligatures: Floss tied around teeth to stabilize the dam.
- Wedges: Inserted interproximally to secure the dam and retract gingiva.
- Proprietary Bands (e.g., Wedjets®): Small rubber bands that hold the dam between contact points.
- Pinching Technique: The dam is stretched and pinched through tight contact points for stability.
Placement Technique
The standard procedure for applying a rubber dam involves the following steps:
- Punch Holes: Create clean, appropriately sized holes corresponding to each tooth’s size and position.
- Try in the Clamp: Attach floss to the clamp to retrieve it if dropped.
- Position the Clamp: Place it on the tooth using forceps, either alone (wingless) or with the dam attached (winged).
- Apply the Dam: Stretch over adjacent teeth using floss to ease it through contact points.
- Secure Anteriorly: Use one of the stabilization methods mentioned earlier.
- Position Frame: Attach the frame to maintain tension and visibility.
- Add Comfort Measures: Place a gauze or napkin under the dam on the patient’s chin to prevent pressure discomfort.
When working with caustic materials or in cases where leakage is possible, apply a rubber dam sealer (e.g., OraSeal®) around the margins to prevent fluid seepage.
Removal of the Rubber Dam
After completing the procedure:
- Remove all clamps, ligatures, and other attachments.
- Cut interproximal septa using scissors.
- Carefully stretch and remove the dam from the mouth.
- Inspect to ensure that no fragments of the dam remain between teeth.
Airway Protection
A crucial function of isolation is to safeguard the patient’s airway during dental procedures. When fitting crowns, bridges, inlays, or performing endodontic treatments, there is a risk of aspiration or swallowing of instruments and materials. The rubber dam provides an effective barrier against such hazards. In cases where a dam cannot be used (e.g., limited access or patient intolerance), alternatives such as gauze screens, butterfly sponges, or throat shields should be employed to provide some level of airway protection.
Gingival Retraction
Gingival retraction is essential when preparing subgingival margins or taking impressions. It involves temporarily displacing the gingival tissues away from the tooth structure to expose the cervical margin clearly. Effective retraction ensures precise impression taking and accurate restoration fit.
Retraction Cords
Retraction cords are thin threads or braids placed into the gingival sulcus using a cord packing instrument. They absorb moisture, control bleeding, and gently push the gingiva laterally. Many cords are impregnated with astringent or vasoconstrictive agents such as adrenaline or aluminium chloride to control bleeding and fluid seepage.
Key points for cord placement:
- The cord should fit snugly but not excessively tight.
- No portion of the cord should protrude from the sulcus (“no tag hanging out”).
- Leave in place for several minutes before impression taking.
- Braided cords are preferred over twisted ones for better handling.
In cases of excessive bleeding, chemical haemostatic agents such as ferric sulfate may be applied.
Astringent Pastes (Expasyl™)
Expasyl™ is a paste containing aluminium chloride, used as an alternative to retraction cords. It provides mechanical and chemical retraction while minimizing tissue trauma. The paste is applied into the sulcus and allowed to act for 1–2 minutes before rinsing away. It is particularly beneficial when the preparation margin lies at or slightly below the gingival level. For deeper subgingival margins, traditional cord methods remain superior.
Electrosurgery in Gingival Management
Electrosurgery involves the use of controlled electrical current to cut or coagulate soft tissues. It is indicated when restorative margins extend subgingivally and mechanical retraction alone is insufficient. Electrosurgery can remove gingival overgrowth, reshape tissue contours, and improve visibility and access for impression taking or restoration placement.
Applications
- Exposure of subgingival margins.
- Crown lengthening (when minimal bone removal is needed).
- Management of hyperplastic gingiva.
When performing electrosurgery, care must be taken to avoid excessive heat generation that could damage underlying bone or cause tissue necrosis. Adequate cooling, short activation times, and precise electrode control are essential for predictable results.
Modern Alternatives and Innovations
The principles of isolation have evolved with technology. Modern dental practice includes innovations designed to improve comfort, efficiency, and compliance.
Rubber Dam Alternatives
Devices such as Isolite® or DryShield® integrate suction, bite block, and retraction in one system, offering partial isolation with improved patient comfort. While they do not replace the traditional rubber dam for high-risk procedures, they are useful for restorative or preventive treatments where full dam placement is impractical.
Digital Dentistry and Isolation
As digital impression systems become more common, moisture control becomes even more critical. Intraoral scanners are sensitive to reflective surfaces and fluids, making isolation a prerequisite for accurate digital data capture.
Conclusion
Isolation and moisture control are integral components of restorative dentistry, directly influencing the quality, durability, and safety of dental treatments. From traditional cotton rolls to sophisticated rubber dams and advanced absorbent materials, the clinician has a wide array of tools available to achieve a dry and controlled operating field. Proper selection and application of these techniques not only enhance restorative outcomes but also elevate the standard of patient care.
A comprehensive understanding of isolation methods allows the dental professional to approach each case with confidence, adapting to anatomical, procedural, and patient-specific challenges. In the modern clinical environment—where adhesive dentistry and infection control are paramount—the mastery of isolation and moisture control is not merely a procedural skill but a hallmark of clinical excellence.
References
- Mount, G. J., & Hume, W. R. (2005). Preservation and Restoration of Tooth Structure (2nd ed.). Knowledge Books and Software.
- Craig, R. G., & Powers, J. M. (2002). Restorative Dental Materials (11th ed.). Mosby.
- Bailey, J. S., & Barghi, N. (2017). “The Role of Isolation in Adhesive Dentistry: Techniques and Clinical Significance.” Journal of Esthetic and Restorative Dentistry, 29(4), 243–250.
- Sturdevant, C. M., Roberson, T. M., Heymann, H. O., & Swift, E. J. (2013). Sturdevant’s Art and Science of Operative Dentistry (6th ed.). Elsevier.
- Ritter, A. V., Swift, E. J., & Heymann, H. O. (2023). Sturdevant’s Art and Science of Operative Dentistry (8th ed.). Elsevier.
- Nash, R. W., & Wilder, A. D. (2011). “Rubber Dam Isolation: A Forgotten Technique Revisited.” Operative Dentistry, 36(3), 243–249.
- Hill, E. E., & Rubel, B. S. (2008). “Do Dental Isolation Techniques Matter? A Review of Evidence.” Operative Dentistry, 33(1), 50–55.
- Cohen, S., & Hargreaves, K. M. (2016). Pathways of the Pulp (11th ed.). Elsevier.
- Rosenstiel, S. F., Land, M. F., & Fujimoto, J. (2015). Contemporary Fixed Prosthodontics (5th ed.). Elsevier.
- Shillingburg, H. T., Sather, D. A., & Wilson, E. L. (2012). Fundamentals of Fixed Prosthodontics (4th ed.). Quintessence Publishing.
- Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2016). Oral & Maxillofacial Pathology (4th ed.). Elsevier.
- Magne, P., & Belser, U. C. (2002). Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Quintessence Publishing.
- McDonald, R. E., & Avery, D. R. (2015). Dentistry for the Child and Adolescent (10th ed.). Elsevier.
- Baldissara, P., Comba, A., Scotti, N., & Michelotto Tempesta, R. M. (2020). “Effectiveness of Different Isolation Techniques on Bond Strength and Microleakage: A Systematic Review.” European Journal of Dentistry, 14(1), 123–132.
- Herman, J. E., & Herman, M. F. (2019). “Gingival Retraction Techniques for Crown and Bridge Impressions.” Journal of Prosthetic Dentistry, 122(6), 547–553.
- European Society of Endodontology (ESE). (2019). Quality Guidelines for Endodontic Treatment: Consensus Report. International Endodontic Journal, 52(12), 174–197.
- American Dental Association (ADA). (2021). Clinical Practice Guidelines: Restorative Dentistry – Infection Control and Field Isolation. ADA Publishing.
- Bland, P. S., & Luther, F. (2022). Contemporary Operative Dentistry: Principles and Techniques. Oxford University Press.